A full scope of the care teams available at NewYork-Presbyterian. Our experts are available to provide top-tier healthcare with a holistic approach.
Our Services
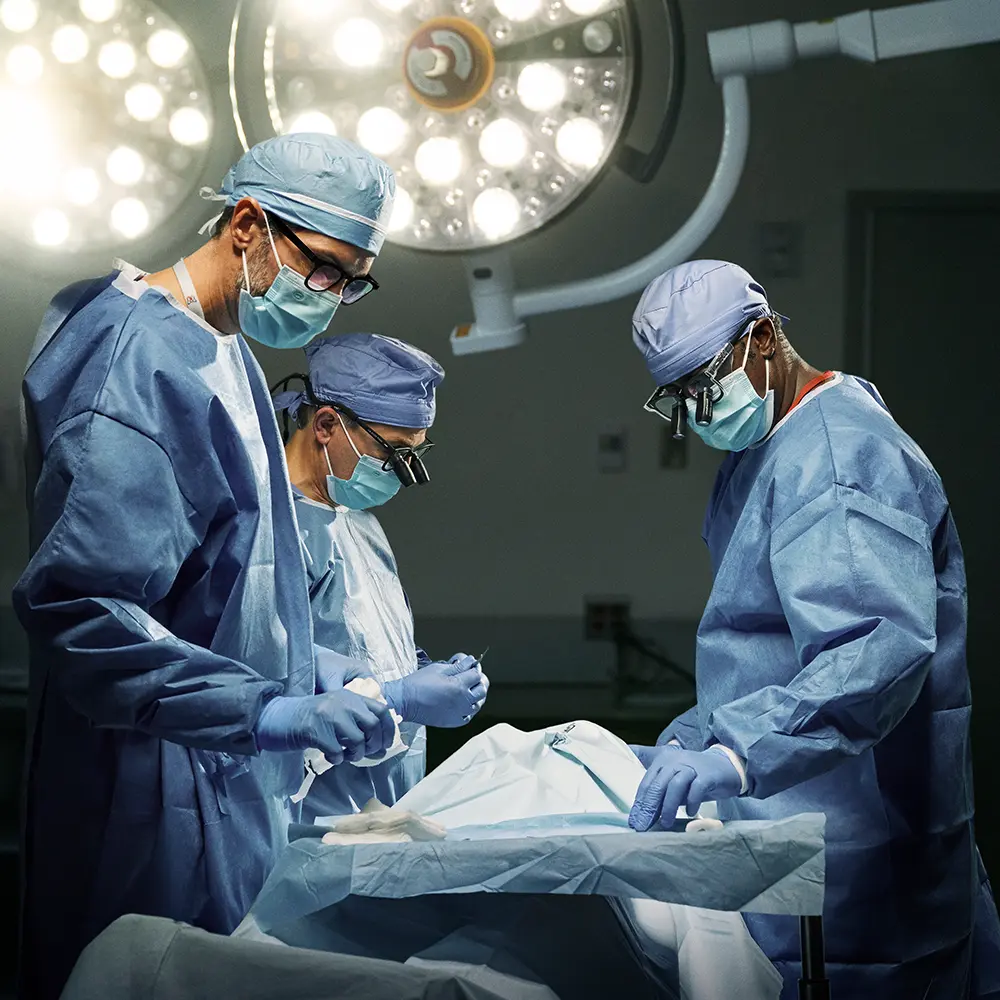
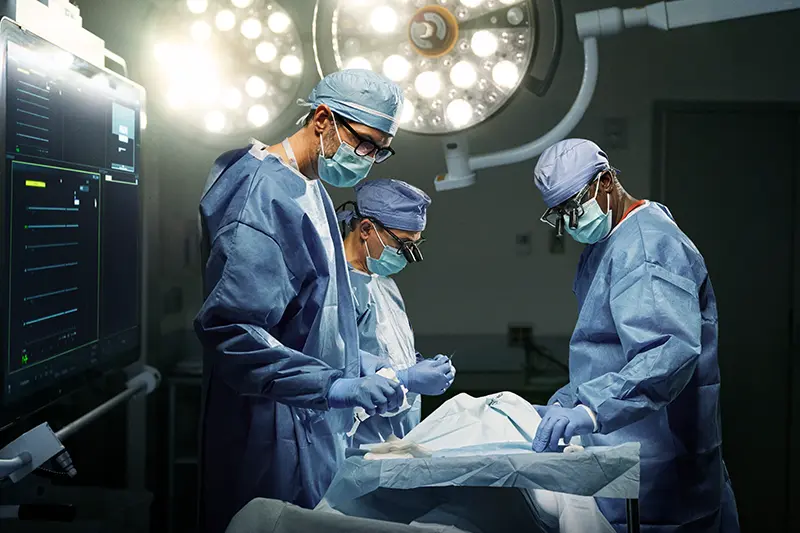
NewYork-Presbyterian offers a large portfolio of healthcare services. These services, categorized by the area of medicine they fall under, relate to the diagnosis, prevention, and treatment of diseases, conditions, and impairments.
Go to:
Featured areas of care
Our digestive care team is experienced in diagnosing and treating a wide array of digestive disorders.
Patients come from around the world to meet with NewYork-Presbyterian cardiovascular experts to treat both common and complex heart conditions.
We offer services for an array of conditions, from headaches to brain tumors, and everything in between.
NewYork-Presbyterian's transplant program is one of the country’s most experienced, innovative, and established programs.
NewYork-Presbyterian orthopedic services treat musculoskeletal disorders such as sports-related injuries, degenerative bone diseases, and spinal injuries and deformities.
NewYork-Presbyterian healthcare experts provide top-tier services to children and adolescents.
NewYork-Presbyterian research and clinical care consistently provides excellent behavioral health programs and service options.
These services include both physical and occupational therapy for musculoskeletal injuries and diseases, burns, stroke, severe trauma, and heart and lung diseases.
The NewYork-Presbyterian vascular medicine team offers advanced diagnostic, preventative, and therapeutic services for vascular disorders that affect blood flow through the arteries and the veins.
NewYork-Presbyterian women’s health teams offer care for patients at every phase of their life, from their childbearing years to menopause and beyond. This includes comprehensive care for every aspect of women’s health.
Looking for symptoms?
All areas of care
- Allergy & Immunology
- Anesthesiology
- Blood Disorders (Hematology)
- Aortic Disease
- Breast Centers
- Cancer Care
- Cardiac Surgery
- Colon and Rectal Surgery
- Congenital Heart Disease
- Coronary Artery Disease
- Dental, Oral and Maxillofacial Surgery
- Dermatology
- Diabetes and Endocrinology
- Digestive Diseases
- Ear, Nose, and Throat (Otolaryngology – Head & Neck Surgery)
- ECMO (Extracorporeal membrane oxygenation)
- Electrophysiology
- Emergency Medicine
- Endocrine Surgery
- Express Care
- General Cardiology
- General Surgery
- Geriatrics
- Hand Surgery
- Heart
- Heart Failure
- Heart Inflammation
- Infectious Diseases/International Medicine
- Integrative Health and Wellbeing Program
- Intra-Hospital Consults
- Internal Medicine
- Interventional Cardiology
- Men's Health
- Nephrology (Kidney Disease)
- Neurology & Neurosurgery
- Nutrition
- Och Spine
- Ophthalmology (Eye)
- Pain Medicine
- Palliative Care for Adults
- Pathology
- Pediatrics
- Plastic Surgery
- Pregnancy & Maternity Care
- Preventive Medicine and Nutrition
- Primary Care
- Psychiatry and Behavioral Health
- Pulmonary Hypertension
- Pulmonology
- Radiation Therapy
- Radiology
- Rehabilitation Medicine
- Rheumatology
- Thoracic Surgery
- Trauma Care
- Urology
- Valvular Heart Disease
- Vascular Medicine
- Video Visit
- Virtual Urgent Care
- Weight Loss Surgery
- Women's Health
- Women's Heart Disease
The transplant program at NewYork-Presbyterian Hospital is one of the country’s most experienced, innovative, and established programs.
Our orthopedic surgeons combine surgical expertise with pioneering clinical and basic research in stimulating bone and tissue repair and total joint reconstruction.
Departments and Centers
Centers are specialized to focus on the prevention, diagnosis, and treatment of a specific ailment or area of healthcare.
- Ambulatory Care Network
- Avon Foundation Breast Imaging Center
- Black Liver Health Initiative
- Borderline Personality Disorder Resource Center
- The Burn Center
- Center for Acute Respiratory Failure
- Center for Advanced Digestive Care
- Center for Autism and the Developing Brain
- Center for Eating Disorders
- Centers for the Performing Artist
- Center for Youth Mental Health
- Community Programs and Services
- Craniofacial Centers
- Dalio Center for Health Justice
- The Endobronchial and Surgical Lung Volume Reduction Center
- Health Navigator Program
- Hyperbaric Oxygen Therapy
- Iris Cantor Men's Health Center
- Integrative Health and Wellbeing Program
- Men's Health
- Military Family Wellness Center
- Multidisciplinary Amyloidosis
- Spiritual Care
- Price Family Center for Comprehensive Chest Care
- Social Work
- Specialty Pharmacy Program
- Support Groups
- Women At Risk

Digital Health
With our digital health services, you can access many of the same healthcare services offered in our hospitals right from your home.



