
Andree Brown

Andrew Solomon

Andrew

Ashley Windle

Balogun Safurat

Belky Aguilar

Benjamin Carey

Bella

Brandon

Bill Doyle

Bob Ward

Britt Sinha

Catherine Hughes

Cherie Aimee

Chloé

Chris Conroy

Chris Marshak

Chris Molnar

Cianah

Daniel Jacobs

Dan Levinson

Davarn Wright

Dena Alsawah

Ebony Boyd

Eileen O'Donnell
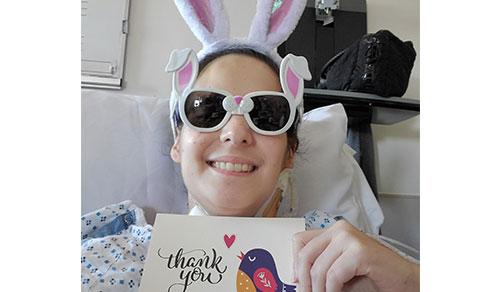
Eliana

Elias Miro

Emily Gorsky

Eric Polans

Evan Kuller

Eve McDavid

Evy Libien

Gavin Deo

Gabby Mansour

Geniene Dillon

Geoffrey Donaldson

Gianna Paniagua

Isabella

Isaac Overson

Jack

Jack Bierwirth

Jack

Jackie Alumno

Jackie Snyder Allen

Jake

Jenna

Jerry Cahill

Jill Vallaro

Jodi Brooks

John O'Brien

Jorge Vicente

Joseph Ania

Julia and The Callas

Julianna Reid

Juliana Zeolla’s

Karin Satrom

Katina Ansen

Kayleigh

Kelly Boyle

Kelly Maggie

Keiran Holohan

Kylie

Lana Guerro

Lance McGinnis

Lauren Kuratko

Leni

Letitia Thomas

Lily

Liz Cabrera

Luis Baez

Lyndsey McLaughlin
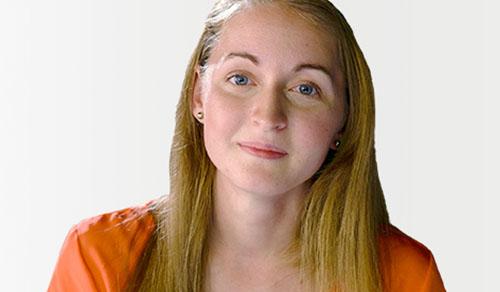
Maddison Wells

Manuel Greco

Matthew S.

Meline Dickson

Melissa Barvels

Michael Cairl

Michael McGuire

Michelle Ellerbe

Miles R.

Mike Cannon

Nancy Jarecki

Nandar Godoy

Nick Masson

Nicole Monzietti

Neil

Nile

Oswald Peterson

Owen

Patricia Anderson

Patrick Hellen

Patti Murillo-Casa

Peter Ciaccia

Peter Reikes

Rachel Rothman

Ramit Malhotra

Raymond Morales

Richard Mandaro

Robbie Magat

Ron Wuaten

Sandy Tonegawa

Sara Musikoff

Selma Rosenbloom

Seth Grumet

Simone Barton

Skylar

Steven Dampf

Synique

Taylor Brown

Toba

Tom Myers

Tony Correa

Trevor MacMeekin

Vanessa Mallilo

Yeniset Estrella




