Pediatric Interventional Cardiology
In July 2020, interventional cardiologists at New York-Presbyterian Morgan Stanley Children’s Hospital were the first in New York State to implant the Alterra adaptive prestent, which allows implantation of transcatheter pulmonary valves in patients with large right ventricular outflow tracts.
With expertise in percutaneous patent ductus arteriosus closure in infants, interventional cardiologists at NewYork-Presbyterian Komansky Children’s Hospital were the first in Manhattan to perform catheter-based closures in preterm infants <1.5 kg.
From 2016 to 2019, our interventional cardiologists performed 5,246 pediatric and adult catheter procedures.
Many of the pediatric interventional procedures that have become the standard of care worldwide were developed by interventional cardiologists at NewYork-Presbyterian. Today, treatments for many CHDs are moving from our operating room to tour pediatric catheterization laboratories. Patients with CHD, from newborn to adult, benefit from the full range of diagnostic and therapeutic transcatheter interventions. Under the leadership of Dr. Alejandro Torres at NewYork-Presbyterian Morgan Stanley Children’s Hospital and Dr. Ralf Holzer at NewYork-Presbyterian Komansky Children’s Hospital, New York Presbyterian interventional cardiologists perform all types of device closure techniques, balloon valvuloplasty procedures, balloon angioplasty, stent implantation and evaluation and therapeutic procedures for pulmonary hypertension.
In the last decade, major technologic achievements have been made in the field of pediatric interventional cardiology including advanced imaging modalities such as 3D echocardiography, computed tomography (CT), MRI, and rotational 3D angiography to prepare for and guide complex transcatheter interventions.
Transcatheter Pulmonary Valve Replacement
In 2007, interventional cardiologists at NewYork-Presbyterian Morgan Stanley Children’s Hospital performed the first catheterization-based pulmonary valve replacement in New York as part of the first FDA trial in the United States involving transcatheter valve placement for CHD. Until that time, replacing a faulty pulmonary valve could be done only with open-heart surgery. This procedure has evolved into a viable alternative to surgical valve replacement, allowing the patient’s pulmonary valve to be replaced nonsurgically and decreases the number of open-heart surgeries a patient with CHD may need over a lifetime. Transcatheter pulmonary valve implantation is now performed at both NewYork-Presbyterian Morgan Stanley Children’s Hospital as well as NewYork-Presbyterian Komansky Children’s hospital.
NewYork-Presbyterian is the primary referral hospital for transcatheter pulmonary valve replacement in the greater New York City area. Over the last decade, our interventional cardiologists have performed >150 transcatheter valve replacement procedures in children and adults with congenital heart disease.
Percutaneous Patent Ductus Arteriosus Closure
Children with congenital heart disease often require medical treatment or a cardiac catheterization procedure to close the ductus arteriosus. Preterm infants are especially vulnerable. With expertise in percutaneous patent ductus arteriosus (PDA) closure in infants, interventional cardiologists at NewYork-Presbyterian Komansky Children’s Hospital were the first in Manhattan to perform catheter-based closures in preterm infants <1.5 kg — the procedure is currently performed at both NewYork-Presbyterian Morgan Stanley Children’s Hospital and NewYork-Presbyterian Komansky Children’s Hospital.
Catheter-Based Interventions
Pediatric interventional cardiology procedures available at NewYork-Presbyterian’s Congenital Heart Center include:
- Transcatheter valve implantation (pulmonary valve, tricuspid valve, and others)
- Stent implantation and/or balloon angioplasty to open narrowed arteries and systemic and pulmonary veins, pulmonary arteries, aorta, and other vascular structures
- Recanalization of completely occluded vessels or atretic valves through radiofrequency perforation
- Device closure of atrial and ventricular septal defects
- Balloon valvuloplasty of all cardiac valves (aortic, pulmonary, mitral, tricuspid)
- Insertion of Impella Ventricular Support Systems for left and right ventricular dysfunction
- Atrial septoplasty for patients with severe pulmonary hypertension and on extracorporeal membrane oxygenation (ECMO)
- Balloon atrial septostomy to improve oxygen mixing within the heart
- Percutaneous patent arterial duct closure
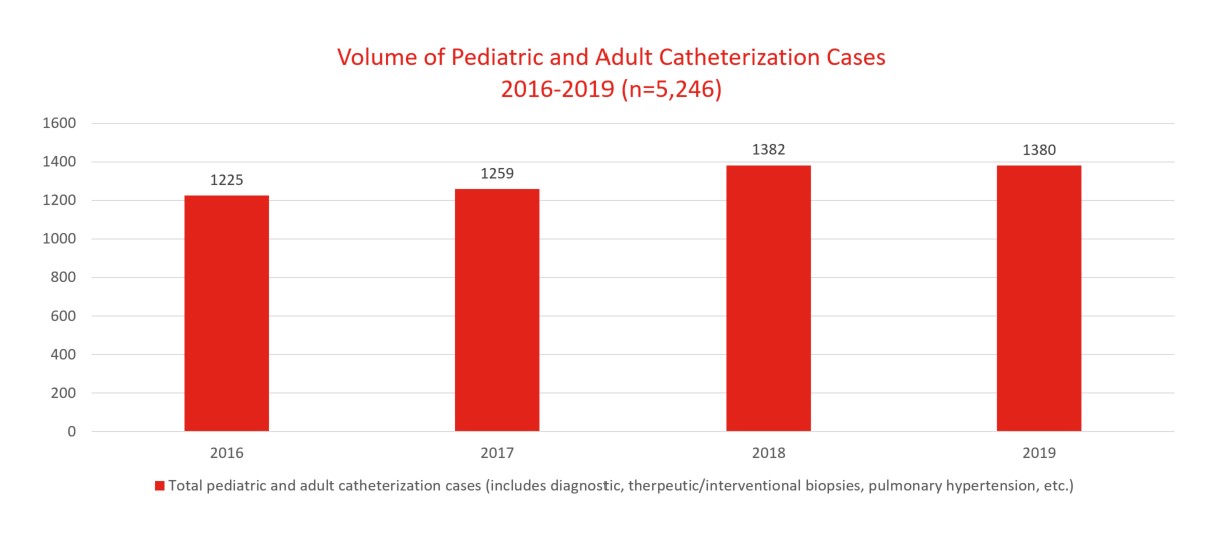
Source: Society of Thoracic Surgeons (STS) National Database 2016-2019.
Pediatric Electrophysiology
Under the direction of Dr. Leonardo Liberman, our electrophysiology services provide diagnosis and treatment of heart rhythm disorders in infants, children, and young adults, with and without CHD. We have performed more than 1,000 invasive procedures in the last decade and our acute success rate in curing arrhythmias is greater than 95%. Pediatric ablation procedures are performed in our state-of-the-art electrophysiology labs equipped with technology to create 3D images of the heart in real-time, minimizing risks to patients and improving the likelihood of eliminating the arrhythmia.
For pediatric patients who are at risk for sudden cardiac arrest, Dr. Eric Silver, Director of the Pediatric Device Implantation program and an active researcher and instructor at NewYork Presbyterian/Columbia, has expertise in clinical cardiac electrophysiology, implanting pacemakers, defibrillators, or loop recorders to help even the littlest of hearts keep the beat.



