Adolescent Bariatric Surgery
Severe obesity is a serious medical problem that can affect the health and wellbeing of children and adolescents. For young people with severe obesity who are unable to achieve or maintain adequate weight loss with conventional approaches, bariatric (weight loss) surgery may offer the best opportunity for successful and lasting weight reduction.
At the Children's Hospital of New York, multidisciplinary teams of weight loss specialists provide bariatric surgery as part of a comprehensive, long-term weight management program for pediatric patients with severe obesity. Our centers are among only a handful in the U.S. approved to offer weight loss surgery to young patients. Our experts in pediatric gastroenterology, surgery, endocrinology, nutrition, mental health, and other specialties work together to help children and adolescents achieve and maintain their weight loss for health and quality of life.
The American College of Surgeons has accredited NewYork-Presbyterian Morgan Stanley Children’s Hospital as an Adolescent Center for bariatric surgery with the highest possible designation – the first program to be so named in New York State and one of only six nationwide. NewYork-Presbyterian/
Obesity and Health Risks
Obesity is an excess of body fat, which is defined as a body mass index (BMI) above 30. Severe obesity is generally defined as being at or above 120% of the 95th percentile for age-adjusted BMI on their growth chart. Children with obesity are more likely to be obese as adults, and obese adults have a higher risk for developing metabolic disorders including type 2 diabetes, high blood pressure, sleep apnea syndrome, and high cholesterol and triglycerides.
Bariatric surgery has been shown to reverse or dramatically improve many of these comorbidities.
About Our Program
At the Children's Hospital of New York, multidisciplinary teams of weight management specialists provide comprehensive care to adolescents with severe obesity. Candidates for surgery typically have a BMI greater than 40, or a BMI greater than 35 with obesity-related medical conditions. Together the Centers have provided metabolic and bariatric surgical care to over 500 children and adolescents since 2005.
Young patients come to our centers in some cases already diagnosed with insulin resistance, hypertension, irregular periods, fatty liver disease, high cholesterol levels, or other conditions associated with their obesity. These patients undergo rigorous education and a lengthy program of multidisciplinary evaluation to determine whether bariatric surgery is appropriate for them.
Our multidisciplinary weight management teams include experts in pediatric gastroenterology, surgery, endocrinology, nutrition, mental health, and other specialties. Together, we evaluate your child and customize an effective plan of long-term, personalized care that includes surgery, education, follow-up, and support as your child settles into new routines and habits that encourage lasting weight loss.
Our programs provide the following:
- Health and metabolic screening
- Nutritional guidance, dietary management, and education
- Individualized exercise programs
- Laparoscopic weight loss surgery
- Ongoing follow-up and support
Evaluating Adolescents for Bariatric Surgery
As noted above, adolescent patients must have a BMI greater than 40 or a BMI- greater than 35 with significant associated illnesses or their growth chart equivalents. Not every adolescent, however, is considered a good candidate for weight loss surgery. Since successful weight loss mainly depends on changing eating behavior and activity patterns, our multidisciplinary team evaluates patients monthly for a minimum of six months before scheduling a weight-loss operation. The team looks for patients to make healthy changes in their eating habits, omitting high-calorie drinks and minimizing high-calorie snacks as well as increasing activity. Candidates who meet standard ASMBS pediatric and metabolic surgery guideline criteria and show positive changes in eating and exercise habits may then be offered weight loss surgery.
Types of Bariatric Surgery For Adolescents
We currently offer the following type of laparoscopic bariatric surgery to our adolescent patients:
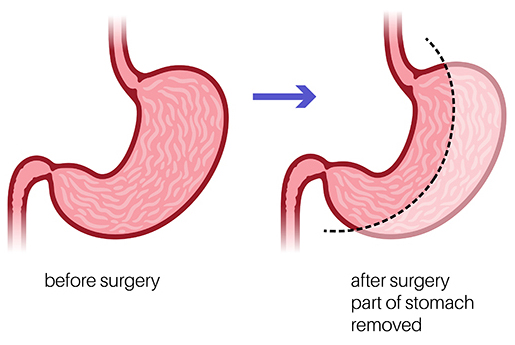
- Laparoscopic sleeve gastrectomy, a procedure for surgical weight loss whereby approximately 80% of the stomach is removed, dramatically reducing the patient's capacity for food intake. This procedure is performed laparoscopically through five small incisions. This surgery has some effect on the body’s absorption of nutrients, and appropriate intake of protein and vitamins after surgery is important.
Long Term Follow-Up
Obesity is a chronic disease, and successful treatment requires long-term follow-up. We continue to follow all patients post-operatively to provide care and to collect results so that others contemplating weight loss surgery can make informed decisions.
Seminars and Support Groups
NewYork-Presbyterian/Columbia University Irving Medical Center’s Center for Metabolic and Weight Loss Surgery offers seminars and support groups to provide adolescent patients with valuable knowledge and comfort before, during, and after bariatric surgery.
Why Choose Us
Nationally Ranked Children’s Hospitals
The Children's Hospital of New York is among the nation's leading centers for the diagnosis and treatment of childhood digestive diseases. They are both major referral centers for complex and rare digestive disorders in infants, children, and adolescents.
Center of Excellence for Bariatric Surgery
The American College of Surgeons Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program (MBSAQIP) has accredited New York-Presbyterian programs as centers of excellence for adolescent bariatric surgery. The American College of Surgeons defines Adolescent Centers and Comprehensive Centers with Adolescent Qualifications as providing complete specialized care for all patients, including those with the most challenging and complex conditions.
Propelling the Field Through Research
The Children's Hospital of New York's pediatric gastroenterologists, endocrinologists, and surgeons are at the forefront of pioneering weight loss techniques and continue to refine bariatric surgery approaches to advance the field. These specialists have conducted pivotal research demonstrating the value of these approaches for improving metabolic disorders such as type 2 diabetes, high blood pressure, and high cholesterol and triglycerides.
As part of a consortium of major children's hospitals, we are also involved in research to carefully study the best uses and outcomes of bariatric surgery in adolescents.