As the U.S. continues to face a major organ shortage, the Center for Liver Disease and Transplantation at NewYork-Presbyterian utilizes innovative methods to expand the donor pool for all ages. When liver transplant candidates come to our center, they have more options, a better chance of receiving a transplant, and experience shorter wait times on the waitlist than other centers in the region. With more than 3,500 liver transplants performed to date, our outcomes continue to meet or surpass national and regional averages.
Leaders in Liver Transplant Innovation and Outcomes
We perform the most liver transplants annually in New York State*
We performed the first fully robotic liver transplant in New York State
We are home to the largest robotic living donor program in the country*
* OPTN, 2025
Comprehensive liver care for adults & children
We offer a full range of services for children and adults with all stages of liver disease, including diagnostic testing, medical treatment, surgery, transplantation, and support. Our surgeons are especially skilled at performing liver transplantation in patients with complex conditions such as hepatitis C virus, HIV, fatty liver disease, and bile duct and liver cancers. NewYork-Presbyterian also transplants two times the volume of patients with polycystic liver disease (PLD) than any other center in the New York area, including Westchester.
We perform liver transplants using organs that come from both deceased and living donors. Our team works with you to determine the best option for your needs, optimizing your overall health while waiting for a liver and working to achieve long-term survival with the highest quality-of-life possible.
Our multidisciplinary liver transplant program offers the following services for children and adults with all stages of liver disease:
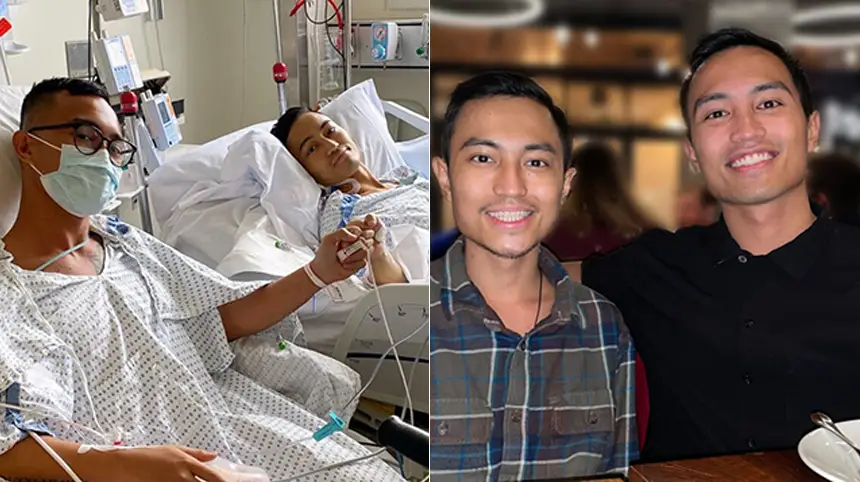
For patients waiting for a life-saving liver transplant, living donor liver transplantation offers many benefits including shorter wait times, faster recovery times, and better outcomes compared to deceased donor liver transplant. Our center has performed more than 500 living donor liver transplantations for adult and pediatric recipients—the second most in the nation—making us one of the most experienced programs in North America with nearly ten times the volume of the next highest center in New York.
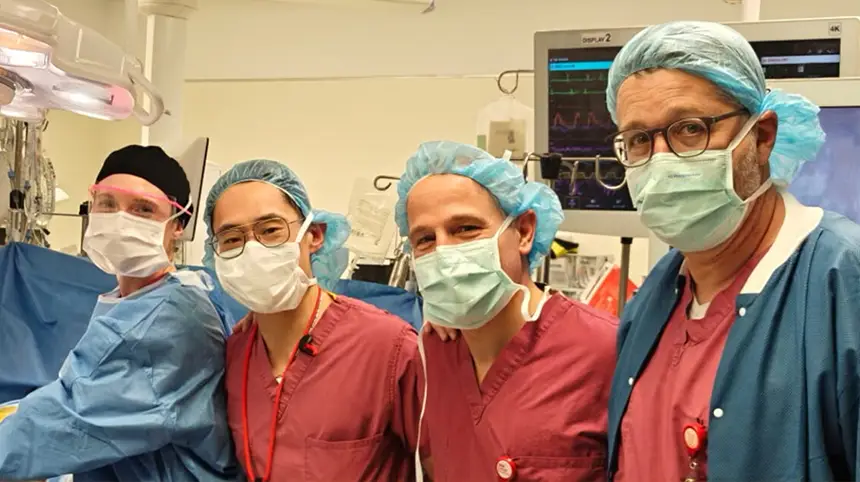
NewYork-Presbyterian was the first to perform a fully robotic liver transplant in New York, and is home to one of only three programs in the country to offer this surgery. This state-of-the-art robotic technology may help patients recover faster, spend less time in the hospital, and avoid surgical complications. All living donor operations are performed using advanced robotic techniques, underscoring our commitment to consistency and innovation.
Learn more about NewYork-Presbyterian's Pediatric Liver Transplant program, one of the largest centers in the nation and one of the only that offer robotic liver surgery in children.
Since the liver has a unique ability to regenerate itself, it can sometimes be used to transplant two different patients. As one of the few centers in the United Sates to utilize split liver transplantation, we are helping to increase the donor pool for children and adults.
Dedicated support for every phase of your care
Liver transplant requires life-long care. Our compassionate team provides personalized care every step of the way—from the uncertainty of waiting for a liver, to the hospital stay and your long-term follow-up care. We partner closely with you and your family with the end goal of helping you spend less time in the hospital and more time living life.
Our team includes a dedicated transplant coordinator, as well as transplant surgeons, hepatologists (liver doctors), gastroenterologists, critical care specialists, nurses and nurse practitioners, pharmacists, psychiatrists, nutritionists, physical therapists, social workers, and financial counselors. We also have support services tailored specifically to living liver donors.
Liver transplant news & stories