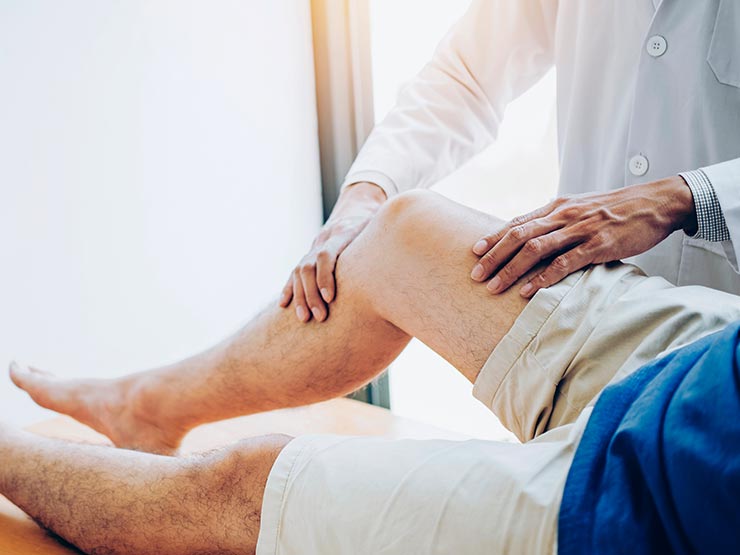
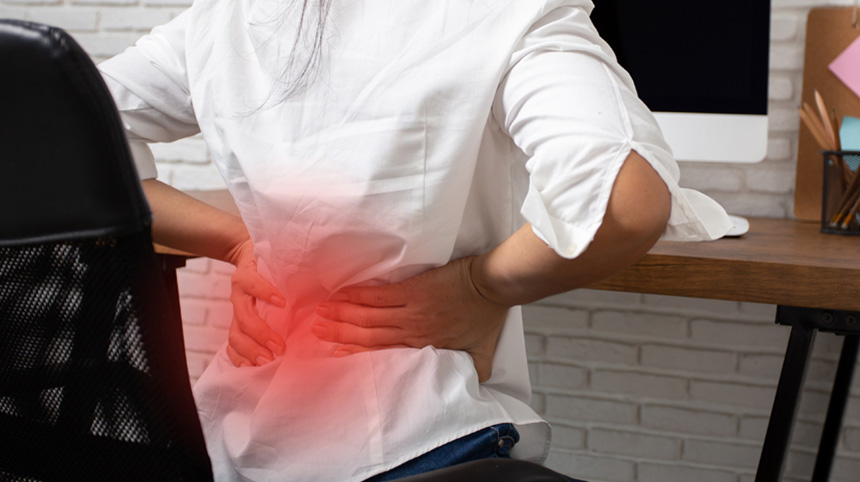
Backed by a team of expert orthopedic surgeons from Columbia, NewYork-Presbyterian is a leading provider of joint replacements in Queens. We perform advanced joint replacements for people with a range of conditions that affect the hips, knees, shoulders, and arms.
In 2017, NewYork-Presbyterian Queens became the first hospital in the borough to establish a comprehensive outpatient joint replacement program. Candidates for the program receive joint replacement surgery with the goal of returning home in under 24 hours and avoiding an overnight hospital stay.