Endoscopy -- the use of a long, flexible tube with a camera at its tip to peer inside a patient -- has been used to help doctors assess and diagnose disorders of the digestive tract. Now "interventional" advances in endoscopy are making it possible not only to see what's going on, but to treat the disorder -- such as opening up obstructions in the ducts linking the liver with the intestine and gallbladder, as well as ducts coming from the pancreas.
Such obstructions may develop as a result of cancer -- including bile duct cancer and pancreatic cancer -- and from acute or chronic pancreatitis (short-term or long-term inflammation of the pancreas). These obstructions can cause significant pain, jaundice (yellowing of the skin), and other symptoms, such as fever and itchy skin, which impair quality of life.
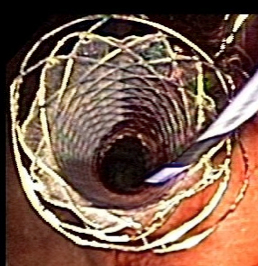
Specialists at the Center for Advanced Digestive Care at NewYork-Presbyterian Hospital/Weill Cornell Medical Center have extraordinary expertise and experience performing the full spectrum of advanced endoscopic procedures to diagnose and treat disorders of the digestive tract.
During endoscopy, a scope is gently inserted down the patient's throat to visualize the area of interest within the digestive tract. Interventional endoscopy takes this approach steps further by incorporating other equipment the doctor can use to open up obstructions (such as cancer tissue, inflammation, or stones), drain fluid, or destroy precancerous tissue. Interventional endoscopy has gone from a technique once used only to diagnose and stage disease, to one we can now use to treat patients.
Contact us
Call for an Appointment
NewYork-Presbyterian
Advanced Interventional Endoscopy



