A Long and Winding Road: Scoping Out Uncharted Territory in the Colon

Dr. Jeffrey W. Milsom
Colon polyps can hide, but they can’t escape the prying eye of the DiLumen™. The DiLumen Endolumenal Interventional Platform (EIP) developed by Jeffrey W. Milsom, MD, Chief of Colon and Rectal Surgery at NewYork-Presbyterian/Weill Cornell Medical Center, and colleagues in the Minimally Invasive New Technologies (MINT) program at Weill Cornell Medicine, is paving the way for dramatic changes in the treatment of many intestinal diseases.
The DiLumen, a dual balloon sleeve that fits securely over a standard endoscope, ensures complete positioning of the scope in the large intestine and assists with optical visualization, diagnosis, and endoscopic treatment. Six years in the making, the device was approved by the Food and Drug Administration in December 2016, and Dr. Milsom and his team began using it in humans last summer. “It is now available for commercial use, manufactured by our industry partner, Lumendi, and its uptake has been rapid,” says Dr. Milsom. “The exciting news is that this endoscopic platform is allowing doctors to perform procedures that were previously either very difficult or impossible to execute. Its main indication for use is for removing very difficult or large polyps inside the intestinal tract.”
Advanced diagnosis and endolumenal procedures are currently limited by the lack of visibility in the colon, especially around flexures and behind folds. As a result, up to 41 percent of polyps are missed during colonoscopy because of poor visibility. The DiLumen improves the visualization provided by current endoscopes and enables better diagnosis and advanced endolumenal therapeutic procedures to be performed for the first time in difficult locations.
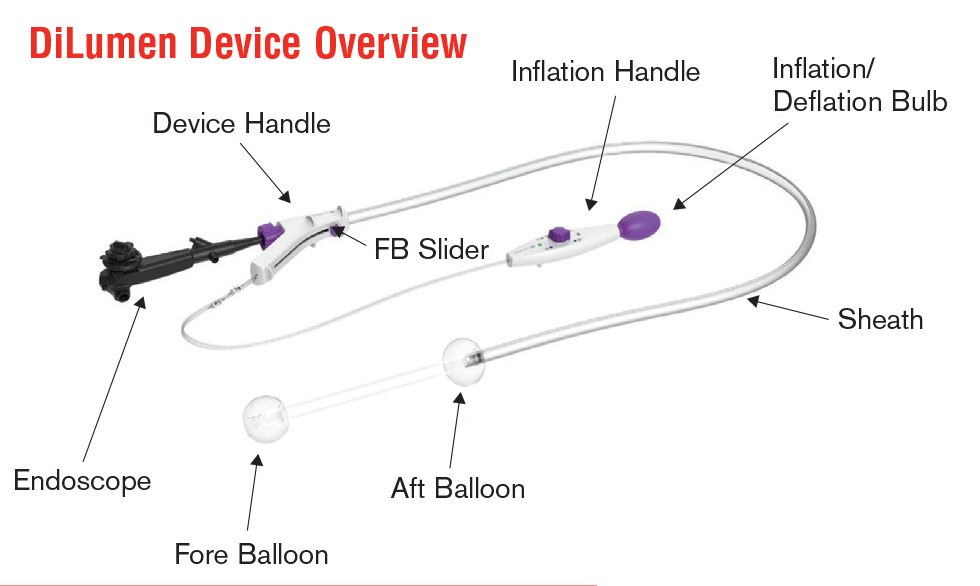
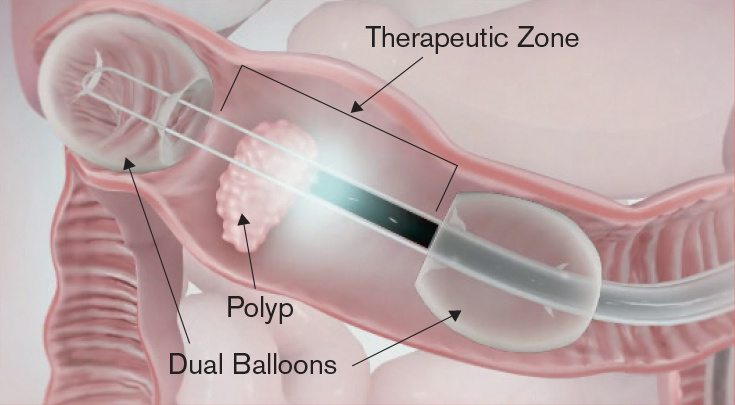
An accessory to an endoscope, the DiLumen device ensures complete positioning of an endoscope in the large intestine and assists with optical visualization, diagnosis, and endoscopic treatment.
As Dr. Milsom explains, the dual balloon system creates a stabilized diagnostic and therapeutic zone within the intestine, allowing clinicians to visualize, manipulate, and treat isolated segments of bowel. “The endoscope is still somewhat free-floating inside the intestine — something like a boat on the water, it bobs up and down,” says Dr. Milsom. “The sheath fits over the endoscope with two balloons on the end of the scope. One balloon is permanently anchored behind the tip. The forward balloon can be advanced about 15 cm beyond the tip of the scope, creating a closed zone between the two balloons.”
Clinicians can precisely extend and retract the forward balloon and manipulate the colon between the two balloons that define the therapeutic zone, reducing the angle of bends and flattening folds in the colon to expose lesions for diagnosis and treatment. “You start to take control of the area,” says Dr. Milsom. “The DiLumen not only appears to be able to be used in all parts of the colon, but it actually makes it easier to navigate through the intestine by virtue of its being a stabilizing device, like a boat moored to a dock. If you can imagine getting to a sharp bend in the colon where you blow up the balloons, that’s what anchors the scope right at that bend. And then you can slide the scope forward and beyond the sheath, making it easier to go around corners and bends.”
The Endolumenal Evolution Continues
Dr. Milsom, his MINT team, and Lumendi have continued to develop additional innovative devices in the evolution of the EIP. In April 2018, the FDA approved the DiLumen C2™. Similar in design to the DiLumen EIP, the DiLumen C2 incorporates two 6 mm diameter tool channels, which accommodate two independent flexible articulating hand instruments.
Dr. Milsom is optimistic about future innovations and their applications to digestive diseases. “The short-term proclamation is that EIP works for the uses in which it was intended, which is always great,” he says. “A lot more needs to be done, however. We want to open up this era of working inside the channel, which is very analogous to what cardiac interventions have done in vascular disease. I think we have even greater potential because we don’t have to arrest the circulation to work inside the channel. The intestine isn’t rushing blood through it, so you don’t have fluid. You can fill the channel with air and it’s safe. You can stabilize the intestine and look directly in with a high-resolution camera. You can also put tools in there. There are so many possibilities that open up.”
According to Dr. Milsom, those possibilities can dramatically impact the way intestinal diseases are treated in the future. “People used to have operations under general anesthesia and a week stay in the hospital,” he says. “We’re now doing outpatient procedures with no incisions, so the patient is able to go home the same day. Local treatment of a tumor may change. By isolating a zone of the intestine, we have the capability of not only surgically removing the lesion, we will probably be able to give intensified chemotherapy, radiation, or immunotherapy directly to the localized site.”
Dr. Milsom stresses that their goals are to make gastrointestinal therapies not only safer, but also less expensive. “If you can apply a local therapy and avoid the need for incisions and hospitalization, these procedures will be safer, more tolerable, and less expensive, and that will decrease healthcare costs,” he says.
Currently the EIP is primarily used for large and difficult-to-access polyps in the colon. “However, this stabilizing device is equally applicable to the upper GI tract, so in the future it will be used for esophageal, gastric, duodenal, bile duct, and pancreatic diseases,” says Dr. Milsom. “Pipeline developments include advanced tools that will provide better surgical capabilities, enabling the development of endolumenal approaches for additional therapeutic areas, such as diverticular disease, stricture, intestinal fistulae, prolapse, volvulus, anastomosis leaks, and early cancers. There will also be other treatments that will emerge — local intensive therapies — not just for cancer, but for conditions such as inflammatory bowel disease.”
Dr. Milsom predicts that endoluminal technology will merge with other types of advanced imaging, including MR CT, which will allow surgeons to look outside of the intestine simultaneously as they look into the channel. “We envision a whole new set of tools and instruments that we’re going to be using,” he says. “At the same time, we’ll be working with other specialties to create new paradigms and a revolution in the way health care is carried out for gastrointestinal problems. This is just the beginning.”
Reference Article
Sharma S, Momose K, Sonoda T, Sharaiha RX. Flexible endoscopic double balloon platform: From concept to human feasibility trial. Gastrointestinal Endoscopy. June 2018, Volume 87, Issue 6, Supplement, Page AB268.
Related Publications





