Cerebral Palsy
Addressing Clinical and Scientific Challenges

Dr. Paulo R. Selber, Dr. Jason B. Carmel, Dr. David P. Roye, Jr., and Dr. Joshua Hyman
The Weinberg Family Cerebral Palsy Center at NewYork- Presbyterian/Columbia University Irving Medical Center serves as a comprehensive program for individuals of all ages with cerebral palsy and a source of important research. “This is the first lifespan center for people with childhood-onset neuromuscular disorders,” says Joshua Hyman, MD, Associate Director of the Weinberg Family Cerebral Palsy Center. “There are a number of places that treat children with cerebral palsy. There are very few centers that treat adults with cerebral palsy, and in this region, no other place treats both children and adults. That’s what makes us unique. As a pediatric orthopedic surgeon, my focus is on the treatment of children, but I am also very interested in what happens to my patients when they become adults.”
“Our physicians and scientists are leading the way in research to provide a better quality of life for people with CP,” says David P. Roye, Jr., MD, Co-Director of Pediatric Orthopedics and Executive Director of the Weinberg Center. “This research stems from clinical practice, with projects that extend from the laboratory to patient care. Our research team maintains the largest CP patient registry in North America, with over 1,000 patients enrolled, and have 15 years of data on over 4,000 patients. We have recently partnered with the CP Research Network to help make this a national resource. Through prospective data collection and retrospective analysis, the team continues to build this important research tool to expand our understanding of CP and related medical conditions in childhood and across the life span.”
Movement Recovery at its Source
Neurologist Jason B. Carmel, MD, PhD, is the Director of the Movement Recovery Laboratory in the Departments of Orthopedic Surgery and Neurology and Scientific Director of the Weinberg Family Cerebral Palsy Center. “Instead of trying to deal with the secondary complications of cerebral palsy — spastic muscles and misaligned joints — we are attacking the problem at its origin, in the brain,” says Dr. Carmel. “My work is about restoring the nervous system connections in order to improve movement.”
Dr. Carmel’s laboratory uses animal models to understand how the brain and spinal cord partner to produce movement. “We seek to understand how neural circuits are compromised by paralyzing injury and how to strengthen brain to spinal connections that are spared by injury,” continues Dr. Carmel. The laboratory uses electrical stimulation of the brain and spinal cord to strengthen movement instructions from the brain and sensory feedback from the spinal cord. Pairing brain and spinal cord stimulation “makes the animals walk better and allows them to better manipulate food when they are eating.”
“We seek to understand how neural circuits are compromised by paralyzing injury and how to strengthen brain to spinal connections that are spared by injury.”
— Dr. Jason B. Carmel
Walking and hand use are two of the activities that people with CP want to recover most. “With this sort of promising intervention, we’ve begun to develop a logic for applying it to people,” says Dr. Carmel. Since brain and spinal cord stimulation are used safely and routinely in clinical practice, this strategy could be quickly moved to clinical trial. Emerging science from Dr. Carmel’s lab and other laboratories around the world is altering conventional thinking that says there is very little that can offer significant recovery for a patient with injury to the central nervous system.
Quantifying Gait Patterns
Supporting the work of both clinicians and researchers will be a new state-of-the-art gait analysis laboratory, being made possible by the recent recruitment of orthopedic surgeon Paulo R. Selber, MD, an international expert in neuromuscular diseases, who also has particular expertise in gait analysis. “Clinical gait analysis can provide objective identification of inefficient gait patterns to confirm a diagnosis and guide treatment selection,” says Dr. Selber, who serves as Co-Director of the Weinberg Family Cerebral Palsy Center. “It is also crucial for orthopedic surgeons to be able to validate functional outcomes following surgery.”
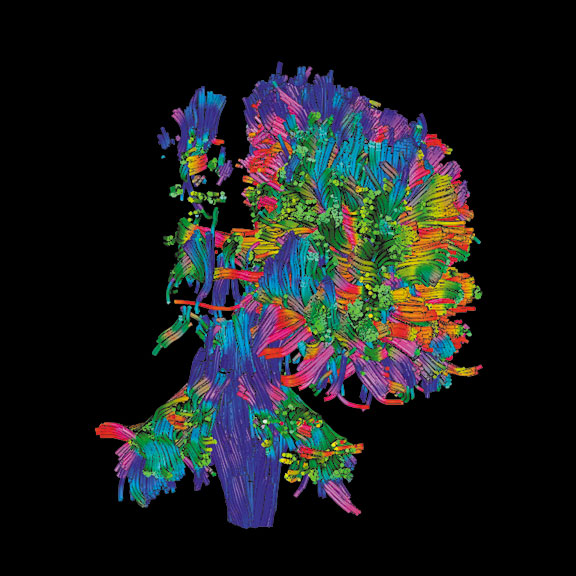
3-D diffusion tensor imaging scan of a rear view of the brain of a 23-year-old with cerebral palsy showing bundles of white matter nerve fibers, which transmit nerve signals between brain regions and between the brain and the spinal cord.
Gait analysis reveals the patient’s cadence, velocity, length of step, and swing time. Information gathered from motion analysis is provided in a series of graphs showing movement, muscle activity, and force production. “Gait analysis is quantitatively and qualitatively validated. However, the interpretations and how you’re going to treat the patient varies depending on who is reading the data,” says Dr. Selber, who has founded gait analysis labs in Brazil and Australia. “Our goal will be to gather motion analysis data for each patient pre- and postoperatively so that we can plan surgical interventions. Each person with CP has different deficits and outcomes will be different from person to person, so I developed a concept called surgical dosing. Gait analysis helps us determine the best surgical dose for each patient.”
Do Genetics Play a Role?
“We know that in the majority of children with CP, onset was intrauterine and prior to the birth process,” says Dr. Roye. “How much of what we call CP is genetic, how much is acquired injury, and how much might be related to other issues?”
The Weinberg Center is collaborating with David Goldstein, PhD, Director, Institute for Genomic Medicine, Columbia University, to study the genetic origins of cerebral palsy. “Over the last few years, studies have revealed that up to 30 percent of people with CP have an associated genetic abnormality,” says Dr. Roye. “Our research seeks to better understand the factors that cause CP and allow us to identify important genetic relationships.” The Weinberg Center’s physicians are now recruiting patients to participate in genetic testing to explore these relationships further.
“ Studies have revealed that up to 30 percent of people with CP have an associated genetic abnormality.”
— Dr. David P. Roye, Jr.
“As we have become more sophisticated in our diagnosis, we recognize that the course of CP may differ depending on the cause,” adds Dr. Hyman. “If I suspect CP, I will always send the patients to neurology to get confirmation, and I'll also send them to genetics. It’s not to determine the underlying genetic cause of their CP, at least it wasn’t, and maybe in the future it will be. Rather, it was to be certain that, in fact, they have CP and not some other underlying problem. I’m hopeful that with increasing genetic knowledge, we’ll be able to cater our treatment better to the patient. It’s on the horizon and we’re seeing developments every year.”



