Pediatric Orthopedics
Influencing Pediatric Spine Care

Dr. Michael G. Vitale
Michael G. Vitale, MD, MPH, Chief of Pediatric Spine and Scoliosis Surgery and Co-Director of the Division of Pediatric Orthopedics, serves as President of the Board of Directors for the Children’s Spine Foundation, and also leads the Children’s Spine Study Group that works to ensure quality research in current treatments. David P. Roye, Jr., MD, Co-Director of Pediatric Orthopedics, and Benjamin D. Roye, MD, also participate in this international study group of some 30 spine surgeons who are focused on improving the care of very young children with scoliosis.
Emphasizing Technology in Nonoperative Scoliosis Treatment
Our pediatric orthopedic surgeons continue to employ techniques and improved technologies for the treatment of early onset scoliosis and adolescent idiopathic scoliosis. These include the MAGEC® (MAGnetic Expansion Control) device, a noninvasive alternative to traditional growing rods that allows surgeons to straighten and correct the spine gradually using a remote-controlled device, as well as the newest generation of “smart” braces. The new braces are lighter, thinner, with a custom-fit that is more respecting of natural balance and mobility. Our surgeons have partnered with a manufacturer to develop a monitor that is placed within the strap buckle of the brace to help track compliance and appropriateness of fit. By using real-time Bluetooth communication to improve brace wear, surgery is less likely and outcomes are much better.
MAGEC allows surgeons to straighten and correct the spine gradually using a remote-controlled device.
Case Study Applying the Magnetic Spine Lengthening Device
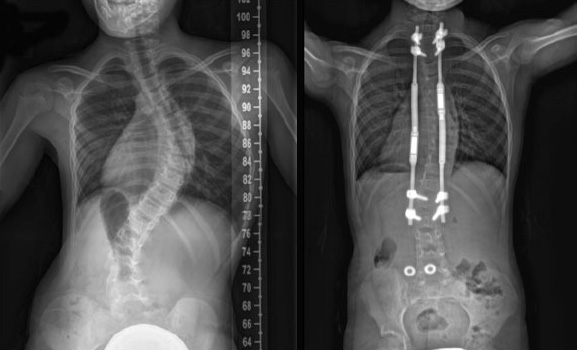
A healthy young girl diagnosed with early onset scoliosis at age 6 seen by Dr. Michael Vitale had a main thoracic curve measuring 61 degrees. Since she was still growing, Dr. Vitale recommended using MAGEC magnetically controlled growing rods, which can be lengthened painlessly and noninvasively during an office visit. Previously, patients with traditional growing rods had to go back to the operating room every six months for lengthenings.
The patient had the surgery, and at her six-week postoperative visit, X-rays showed that the curve had decreased to 31 degrees. The appearance of her back and her overall balance and alignment were drastically improved. Within six weeks of surgery, she was back to school and ready to start playing soccer again.
Leaders in Spinal Muscular Atrophy
Our pediatric spine surgeons have particular expertise in the treatment of scoliosis spinal muscular atrophy (SMA), from young children to young adults, and were among the first in the country to pioneer surgical approaches that are more aggressive in stopping the scoliosis early on and avoiding extensive fusion. Our pediatric spine specialists continue at the forefront nationally, leading the way in novel medical treatments that are transformational, enabling children who were never going to be able to walk to now walk. NewYork-Presbyterian/Columbia was the first institution to pioneer gene-replacement therapy, and an SMA patient here was among the first in the country to receive the treatment.
A multicenter phase 3 clinical trial — STR1VE — is currently underway in infants less than six months old with SMA Type 1 based on gene mutation analysis. The trial will evaluate outcomes that include event-free survival at 14 months of age, and achievement of independent sitting, ability to thrive, and ability to remain independent of ventilator support at 18 months of age.
Cerebral Palsy
Cervical Spinal Stenosis and Spastic Cerebral Palsy

Dr. David P. Roye, Jr., and Dr. Benjamin D. Roye
Dr. David Roye, who is also Executive Director of the Weinberg Family Cerebral Palsy Center at Columbia, has identified a pattern in adult patients with mild to moderate cerebral palsy, who presented with trouble walking and increased spasticity. Dr. Roye and his Columbia colleagues began to screen these patients with X-rays of the cervical spine, discovering that many patients had cervical spinal stenosis (CSS). Although an association with CSS is well-recognized for athetoid/dystonic types of cerebral palsy, there was little information available on CSS in patients with spastic CP. Undertaking a retrospective study drawing on the Weinberg Center’s registry of 6,000 patients, the physicians reviewed 3,000 adults with CP, from 2006 to 2016, looking for diagnoses associated with CSS in cerebral palsy. The results of the study, published in Developmental Medicine and Child Neurology in August 2017, found that of the patients with CSS, 73 percent presented with upper extremity symptoms, 70 percent with ambulation decline, 53 percent with neck pain, and 30 percent with incontinence.
Today, new patients with CP over the age of 35 seen at the Weinberg Center routinely have cervical spine X-rays whether or not they have complaints. Patients in their 40s and 50s who have a reasonably high index of falling, worsening muscle spasms, and urinary bladder malfunction undergo an MRI. By identifying a degenerative process that is thus far undetected, patients can be referred for effective surgical treatments that carry a high success rate.
Expanded Services for Adults with CP
Approximately 90 percent of children with CP now live into adulthood. The Weinberg Center has begun providing the coordination and continuity necessary to ease the transition of teenage patients into adult care. A growing network of Columbia physicians from specialties, including cardiology, rehabilitation medicine, neurology, psychiatry, and urology, provide comprehensive care to patients in this transition.



