Adult Spine

Dr. Lawrence G. Lenke
Chief, Spine Division
Surgeon-in-Chief
Daniel and Jane Och Spine Hospital
Dedicated Facility for Spine Treatment
The Daniel and Jane Och Spine Hospital at NewYork-Presbyterian Allen Hospital provides an integrated, multidisciplinary approach to the treatment of spine disorders. Here, renowned orthopedic spinal surgeons, physiatrists, and pain management specialists offer comprehensive care for patients in a single facility, ensuring the coordination of all aspects of preoperative, intraoperative, and postoperative treatment. The Daniel and Jane Och Spine Hospital features:
-
5 operating rooms custom built for spine surgeries
-
ICU beds attended by spine-specific intensivists
-
Low radiation technology for imaging the entire skeleton
-
Robotics system
-
Real-time OR video feed to observation rooms

Dr. K. Daniel Riew
Co-Chief, Spine Division
Director, Cervical Spine Surgery
Progressive Techniques and Technologies
-
Our surgeons are trained in the most advanced, least-invasive surgical techniques, including microsurgical and endovascular options. For the most complex spinal deformity surgeries – many of which can be performed at only a few hospitals in the world – they use CT imaging data to create 3-D models that they can use before surgery in order to precisely plan the placement of screws and other aligning instruments.
-
Robotic technology is now being used as a tool to enhance positioning accuracy, minimize invasiveness, and reduce radiation exposure to the patient and surgical team during spine surgeries. The bonemounted, miniature robotic system guides the accurate placement of implants, offering surgical tool guidance while leaving the actual procedure in the surgeon’s hands.
Visiting surgeons from all over the world come to the Daniel and Jane Och Spine Hospital to benefit from training by expert surgeons with the knowledge, technique, and resources to treat the most complex disorders and deformities.
Case Studies
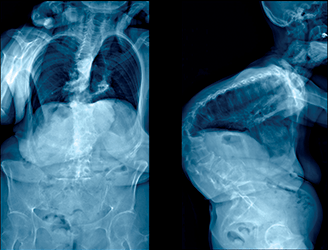
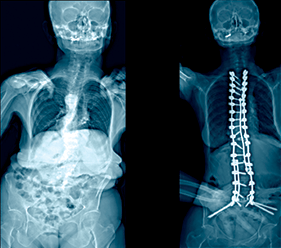
A patient presented with severe kyphosis due to multilevel osteoporotic compression fractures. She was treated with posterior spinal instrumentation and fusion from T2-sacrum with a T11 vertebral column resection in a nine-hour surgery.
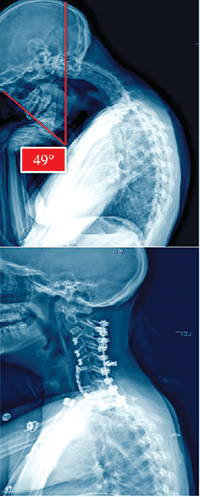
A 28-year-old female with a seven-year history of kyphoscoliosis and dystonia also presented with psoriatic arthritis, ankylosing spondylitis, and cervical dystonia. A three-hour anterior surgery was first performed followed by asymmetric osteotomies to correct the scoliosis at C3-4-5-6-7-T1, with anterior fusion from C2-T1. Posterior osteotomies were then performed in a more than five-hour surgery at all the same levels with a fusion from C2-T2.
The patient is now ambulating normally and expected to resume all normal activities better than she could preoperatively since her alignment is now nearly normal.
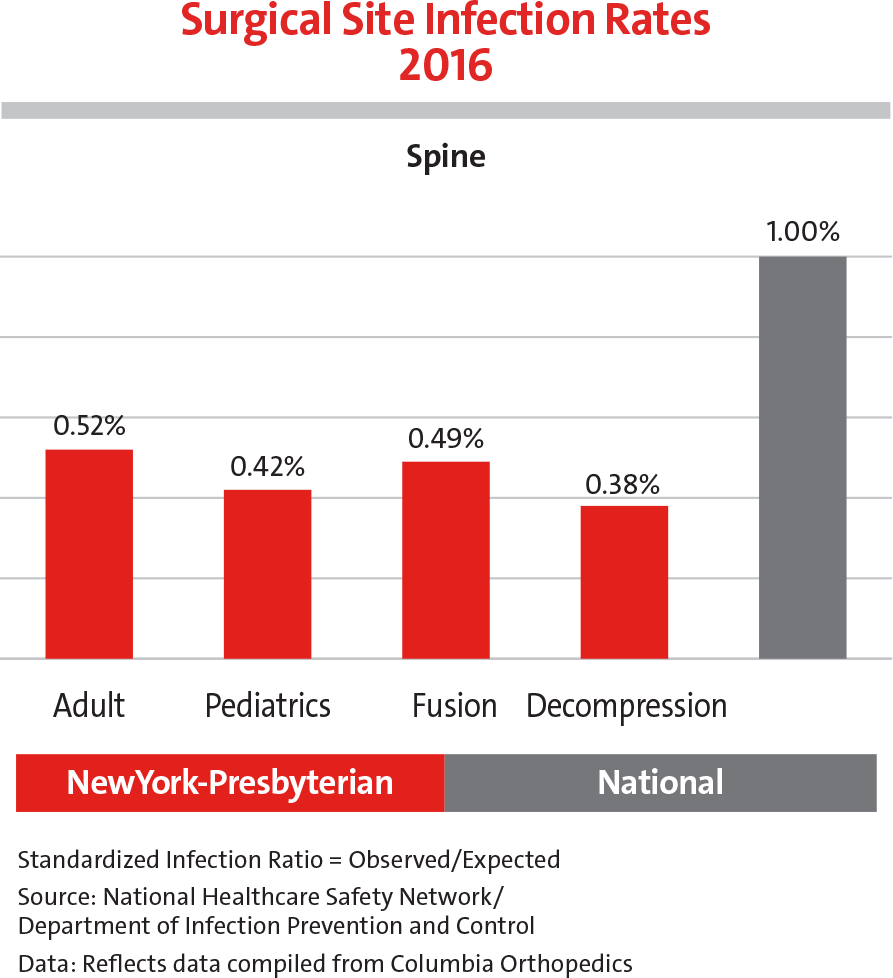
The surgical site infection rate on average for adult and pediatric spine procedures is less than 50% of the national baseline.