Prenatal Diagnosis & Intervention
We have one of the largest and most experienced maternal-fetal medicine teams in the country, with over half of all deliveries designated high-risk or increased risk. The Maternal Fetal Medicine Program at NewYork-Presbyterian Morgan Stanley Children’s Hospital is under the direction of Dr. Lynn Simpson. Fetal Cardiology is under the direction of Dr. Stephanie Levasseur. At NewYork-Presbyterian Komansky Children’s Hospital, the Clinical Maternal-Fetal Medicine Program is directed by Robin Kalish, MD. Sheila Carroll, MD, directs the Weill Cornell Fetal Cardiology Program.
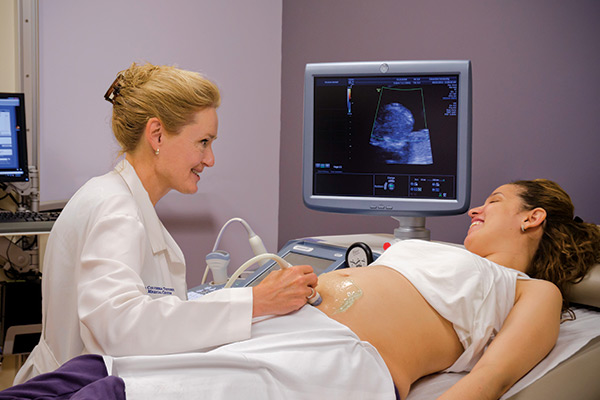
Our Carmen and John Thain Center for Prenatal Pediatrics at NewYork-Presbyterian Morgan Stanley Children’s Hospital and our Fetal Cardiology Program at NewYork-Presbyterian Komansky Children’s Hospital are the only facilities of this kind in the New York area offering comprehensive, multidisciplinary prenatal diagnosis and therapy in conjunction with pediatric subspecialty consultation. We communicate all test results, diagnoses, and specific treatment options with the referring obstetrical team in a timely manner and coordinate a care plan for the patient.
Fetal Cardiac Therapy
In 2018, our fetal cardiology team began providing fetal cardiac intervention, the first in New York to provide this therapy. When a heart defect is suspected in utero, we bring together a core team of high-risk obstetricians, neonatologists, interventional cardiologists, fetal cardiology specialists, pediatric congenital heart surgeons, and other cardiac specialists. Working jointly with our colleagues in maternal-fetal medicine, we precisely diagnose the anomaly, develop a plan for close surveillance, and prepare for surgical intervention and the proper level of care at delivery, ultimately leading to improved outcomes. In cases where fetal therapy is possible, such as for cardiac arrhythmia, collaboration with pediatric cardiologists can maximize our ability to improve fetal health while avoiding complications in the mother.
Twin-Twin Transfusion Therapies
As the number of women having twins has increased, so have the chances of developing a serious pregnancy complication called Twin-Twin Transfusion Syndrome (TTTS). This disorder affects as many as 15 percent of identical twin pregnancies and results from uneven blood flow between the fetuses. Successful treatment of this complex condition requires advanced training and experience available at only a few specialized perinatal centers in the United States. In more than 70 percent of cases, both twins will die if this syndrome is not treated early in pregnancy.
During the years 2015, 2016, and 2017 our Maternal-Fetal Medicine specialists performed more than 60 laser photocoagulation procedures, a minimally invasive laser treatment, which involves coagulating unnecessary and harmful blood connections between the two fetuses. NewYork-Presbyterian is currently the only center in Manhattan that performs the laser photocoagulation procedure.
Twin-Twin Transfusion Syndrome can have a significant impact on the cardiovascular system in twins. It is important that twins with TTTS are thoroughly evaluated for heart problems in utero. An obstetrician may refer a patient for further evaluation and fetal echocardiogram by our maternal-fetal medicine cardiovascular team.



