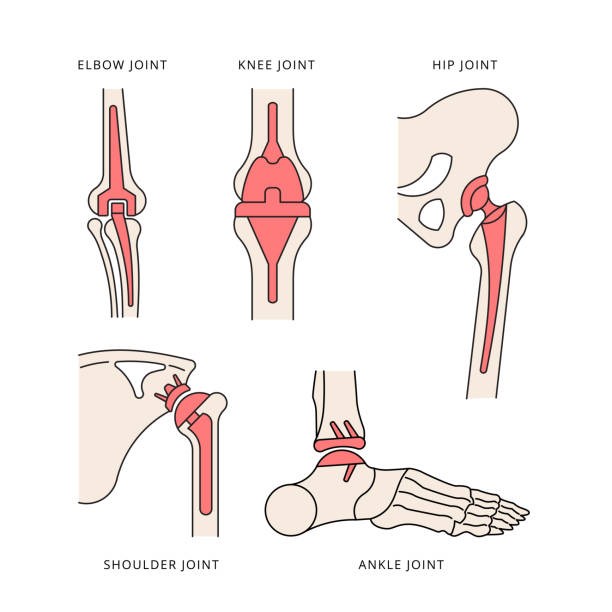
Joint replacement surgery—also known as joint arthroplasty—is one of the most common orthopedic procedures performed in the United States. Patients with severe arthritis, traumatic injuries, or other ailments that cause discomfort and limit their mobility and quality of life may benefit from a joint replacement.
What is Arthroplasty?
What is Arthroplasty?Arthroplasty is an operation to replace all or part of an impaired joint with an artificial joint to reduce pain and improve function. The artificial joint is usually made of metal, ceramic, or durable plastic. This procedure is most often reserved for people in whom nonsurgical treatments—such as physical therapy, medications, injections, and lifestyle modifications—are ineffective for improving their symptoms. Arthroplasty is available for patients in need of a hip, knee, shoulder, elbow, or ankle replacement, with hip and knee replacements being the most common.
Common reasons for joint replacement
Joint replacement surgery is most often used for people with:
- Severe arthritis, including osteoarthritis (a degenerative condition) and rheumatoid arthritis (an autoimmune disease)
- Fractures, such as some hip fractures
- Traumatic injuries from incidents such as falls or motor vehicle collisions
- Joint abnormalities such as hip dysplasia (where the thigh bone does not fit comfortably in the hip socket)
- Avascular necrosis, a condition involving lack of blood supply to the bone
Who needs joint replacement?
People who most commonly receive a joint replacement include:
- Patients with advanced symptomatic arthritis
- Older patients who have sustained some subtypes of hip fractures
- People who have major joint injuries from an accident or fall
- Individuals born with joint abnormalities that cause discomfort and impair function
Types of Arthroplasty (Joint Replacement)
TypesIn the United States, more than a million joint replacements are performed every year. Types of arthroplasty include:
- Total hip replacement, where the ball and socket of the joint are replaced
- Total knee replacement, where all three of the compartments of the knee are replaced
- Partial knee replacement, where only one or two of the three compartments are replaced
- Shoulder replacement, which can be total shoulder arthroplasty (the socket, ball, and stem) or involve the replacement of only certain components
- Elbow replacement, which may involve the entire elbow or only part of the joint
- Ankle replacement (total ankle arthroplasty), which is not as common as the other procedures and is used for severe ankle arthritis that cannot be well treated with other methods
- Carpometacarpal (CMC) arthroplasty is a treatment for thumb arthritis in which a small wrist bone that is part of the CMC joint is replaced with a tendon
Revision surgery is an operation that is done to correct or replace an implant that was previously inserted during a prior surgery but is not functioning well or has worn out over time.
How is Arthroplasty Performed?
ProcedureYou are placed under anesthesia—generally, spinal anesthesia where the extremity is paralyzed and numb but you are awake (but sedated) and not intubated. Arthroplasty is an open surgery, meaning an incision is used to access the joint. The worn cartilage is then removed and replaced with artificial components.
Some joint replacement surgeries can be done using minimally invasive methods, meaning that surgeons will operate through smaller incisions. This may help to preserve the muscles and speed your recovery. For example, minimally invasive hip replacement can be completed through a small incision with implant placement guided by X-ray, and minimally invasive knee replacement can be done through one small incision. Robotic-assisted approaches are also available for some joint replacements, with the surgical robot enhancing the precision of implant placement.
Joint replacement surgery takes about one to two hours, but the duration of your surgery will depend on the type of arthroplasty as well as the complexity of the joint being replaced. Your surgeon will present you with options, discuss which approach may be best for you, and let you know what to expect after your procedure.
Risks to Consider
RisksLike all surgeries, there are certain risks associated with joint replacement surgery, including:
- Infection within the joint and/or the incision
- Damage to the nerves around a joint
- Blood clots
- Joint stiffness or instability
- Problems with the alignment of the new joint, including dislocation
- Scar tissue
- Loosening or wearing down of the implant
You and your doctor can discuss these issues and whether or not you're at an elevated risk.
Preparing for Joint Replacement Surgery
PreparingThere are several ways to prepare for your procedure—some of the following actions are required, while some are suggested.
- Physical exam - You may have a physical exam given by your primary care physician, along with blood tests, an electrocardiogram (which assesses heart function), and a chest X-ray to make sure you’re healthy enough for surgery
- Medications - If you take blood thinners, you will be instructed when to stop taking them before surgery
- Get healthy - Your doctor may advise you to improve your physical condition before surgery, which will help you recover more easily. This may involve losing weight, seeing a dietitian to learn how to follow a healthy diet, scheduling sessions with a physical therapist to improve your strength and flexibility, and stopping smoking.
- Set things up - Get your home set up to make sure it’s as easy as possible to get around once you get back from your procedure. You may wish to cook and freeze meals ahead of time, move items you commonly need so they are within easy reach, practice getting around with a cane or walker if you will have one after surgery, remove any area or throw rugs to reduce your risk of a fall, and/or put in a raised toilet seat.
- Arrange for help - Arrange for someone to take you home after the procedure. If you live by yourself or have special needs, line up someone to help you around at home for several days, or talk with your care team about other post-discharge options.
- Bathing before surgery - Follow your doctor’s orders for bathing before the operation. A special antibacterial wash may be recommended to reduce the risk of infection.
What to Expect after Arthroplasty
After the SurgeryDepending on which procedure you undergo and your other medical conditions, if any, you may go home within a day of your operation or stay in the hospital one to two nights. Your care team will give you all the information you need to take care of yourself after you leave the hospital. It can take several months to completely recover from joint replacement surgery. Your doctor's instructions may advise you to:
- Avoid overexerting yourself - You'll need rest to heal from the operation. Listen to your body. You will need to elevate the affected joint to reduce swelling while you rest.
- Do physical therapy exercises as prescribed - Physical therapy can be critical after surgery. If you have had a shoulder or elbow replacement, you may have occupational therapy. A physical or occupational therapist may visit you while you are still in the hospital. If you’re given exercises to do, make sure to stick closely to the plan that your care team provides. This is essential to ensure you achieve mobility, flexibility, and strength with your new joint.
- Keep your incisions covered and clean - Your care team will give you instructions about how to take care of them and how often to change the dressing if needed. Many modern dressings no longer need to be changed or cleaned at home.
FAQs About Joint Replacement Surgery
FAQsHow long does a joint replacement last?
Your new joint can last 20 years or longer depending on which joint is replaced. Speak with your physician about ways to keep your new joint healthy for as long as possible, such as avoiding certain high-impact activities.
What type of surgery is arthroplasty?
Arthroplasty is an orthopedic surgery used to replace a damaged joint with an artificial joint.
Trust NewYork-Presbyterian for Arthroplasty
If you have chronic pain, stiffness, swelling, or other discomfort in a joint and have found little to no relief from medication, bracing, physical therapy, or other non-surgical treatments, you may be a candidate for joint replacement surgery. The joint replacement team at NewYork-Presbyterian’s Columbia Orthopedics leverages the latest approaches in orthopedic surgery to provide tailored treatment plans and achieve superior outcomes for our patients. .
We offer advanced techniques such as minimally invasive anterior approach hip replacement, robotic-assisted joint replacement surgery, and complex reconstruction to repair or replace a failed or damaged joint replacement. NewYork-Presbyterian's rehabilitation specialists are also part of our team and can help you get ready for your operation as well as support your recovery.
Contact us today to make an appointment and learn how you can start feeling better.