In May 2023, an integrated team of cardiologists and cardiothoracic surgeons at NewYork-Presbyterian/
Dr. Goldstone Outlines the Unique Aspects of a Domino Partial Heart Transplant
NewYork-Presbyterian performs the most transplant surgeries in the United States and was uniquely positioned to pioneer the domino partial heart transplant procedure due to the extensive expertise and training that went into preparing for this moment. Although partial heart transplants have been performed a handful of times in pediatric patients, this was the first time one was done as a domino procedure. The care team established for both patients was comprised of several cardiologists, cardiothoracic surgeons, nurse practitioners, perfusionists, anesthesiologists, and others, under the leadership of:
- Marc Richmond, MD, MS, pediatric cardiologist and Director of the Program for Pediatric Cardiomyopathy, Heart Failure and Transplantation, who led the medical team for both patients pre- and post-operatively
- David Kalfa, MD, PhD, a pediatric cardiothoracic surgeon, Director of the Pediatric Heart Valve Center, and Surgical Director for the Initiative for Pediatric Cardiac Innovation, who performed the domino partial heart transplant, also known as a living allogeneic heart valve transplant
- Andrew Goldstone, MD, PhD, a pediatric cardiothoracic surgeon, Surgical Director of Pediatric Heart Transplantation, and Surgical Director of Pediatric Heart Valve Transplantation, who performed the heart transplant and assisted with the valve transplant
Typically in a domino procedure, one patient undergoing transplant donates one of their explanted but healthy organs to another patient in need of an organ transplant. The organ is explanted from one living transplant candidate and immediately transplanted into a second patient, while the initial patient receives a new organ from a deceased donor. What made the procedure at NewYork-Presbyterian/
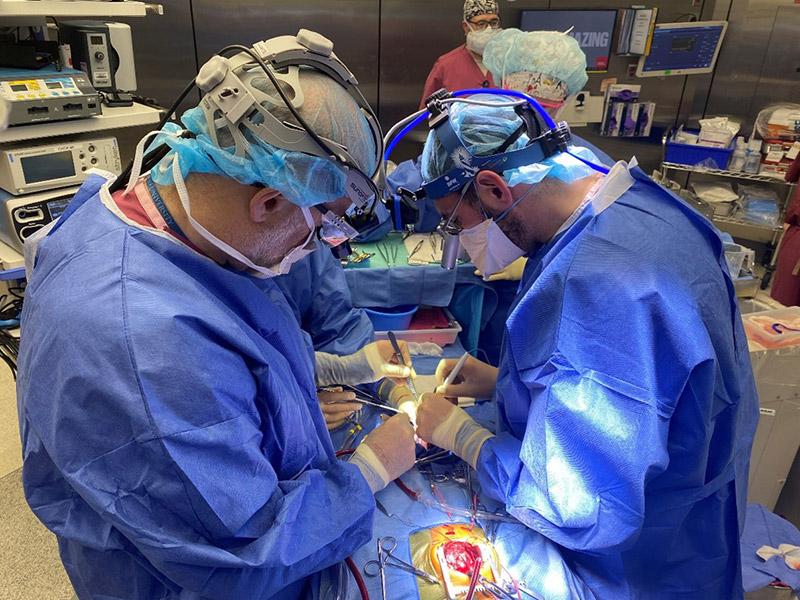
Andrew Goldstone, MD, PhD and David Kalfa, MD, PhD.
“This procedure is truly disruptive,” says Dr. David Kalfa. “These new valves (coming from Mia’s explanted heart) that we implanted in Brooklyn’s heart to replace her dysfunctional valves are living valves and have the potential to grow and self-repair with Brooklyn. Having these living and growing valves is the Holy Grail in pediatric cardiac surgery because none of the current options to replace heart valves in children have a growth potential. They all fail and need to be replaced multiple times with open-heart surgery before the child can reach adulthood. This procedure will transform Brooklyn’s life and quality of life.”
Valve transplants aren’t a completely novel idea; they were previously done in adults in the mid-to-late 1900s. Previously called homovital homografts or allografts, medical science at the time did not allow for longevity of these valve, and thusly surgeons eventually phased out this procedure in adults in favor of xenografts or cryopreserved valves. However, in the intervening decades, infant heart transplantation has become standard therapy with excellent long-term outcomes. That led surgeons to revisit this technique in infants in recent years because the living allogeneic valves can grow with the patients as they age, reducing the need for repeated, invasive surgeries.
“We have decades of scientific evidence supporting whole organ transplant, it’s a great therapy for children that have uncorrectable heart disease,” says Dr. Andrew Goldstone. “There’s currently no available valve replacement surgical prosthesis that will allow you to have a growing valve. And so for children, where we must constantly replace valves, this is truly unique. If the recipient of this continues to show that they have a growing valve, it could completely change the way we treat pediatric heart valve disease.”
The procedure performed at NewYork-Presbyterian/
Identifying the Right Living Organ Donor/Recipient Pair
Identifying the right living donor/recipient pair was the first key step that needed to occur to ensure a successful transplant. Timing was critical as both patients needed to have surgery at the same time and a donor heart needed to be available in that same period.
“We had been planning to do a partial heart transplant to replace Brooklyn’s valves for many weeks because we knew that this was the best option for her”, says Dr Kalfa. “Unfortunately her ventricular function deteriorated too quickly to wait for a donor to become available in time. We got so lucky in terms of timing that Mia got a donor offer and that her parents consented to donate her valves to help Brooklyn”.
Dr. Goldstone received the donor offer for Mia in the early morning hours of a Wednesday, around 2 a.m. “She had been waiting quite a long time,” says Dr. Goldstone. “So it was very exciting that she got a donor offer. Although Mia’s heart muscles were weak, her valves were working normally.”
“I was looking at our case conference list for the next morning where we were going to discuss patients, and I saw Brooklyn’s case on the list,” he says. “That’s when I realized that this one donor heart could actually be the solution for both these patients.”
Marc Richmond, MD, MS
The heart center team reviewed Brooklyn’s case that morning during a multidisciplinary case conference and discussed the options for fixing her valve disease, none of which were ideal. A valve replacement was the best solution for her condition. “She was the only patient that we had identified, at the time, who would benefit from this type of procedure,” says Dr. Marc Richmond. “It was made very clear that not only would she be a good candidate for valve transplantation but that she couldn’t wait.”
Fortunately, Mia’s valves were a size match for Brooklyn and with her receiving a donor heart, her heart would be used to provide new aortic and pulmonary valves for Brooklyn.
After meeting as a team, Dr. Richmond, joined by NewYork-Presbyterian/
Assembling Multidisciplinary Care Teams
Three teams were required to successfully complete the domino transplant – an organ procurement team for the donor heart, a surgical team to implant the new heart and explant the old one, and another surgical team to implant the domino donor valves. “When this idea came out, everyone was on board and everyone put their all into making sure this would happen, from the physicians to the nurses to the perfusionists, literally everybody inpatient and outpatient,” says Dr. Goldstone.
“It took a village to make this incredible procedure happen in such a short amount of time”, said Dr. Kalfa. “This is the very moment that you can see how much a dedicated multidisciplinary team with a strong will to innovate and a passion for caring of the sickest can accomplish. I was so grateful to be part of this team”
The partial heart transplant team was made up of nine people, led by Dr. Kalfa and Emile Bacha, MD, Chief of the Division of Cardiac, Thoracic, and Vascular Surgery at NewYork-Presbyterian/
The full heart transplant team was made up of seven people including Dr. Goldstone and Edward Buratto, MD, PhD, a pediatric cardiothoracic surgeon at NewYork-Presbyterian/
The entire group was pulled together in less than 12 hours. “To see that happen is truly amazing,” said Dr. Goldstone. “That only happens if everybody is totally invested in each patient’s life and wellbeing. That’s something that amazes me and it’s one of the reasons why I love working here – the teamwork is on constant display.”
Beginning the Operations Concomitantly
It was about 15 hours from the time the doctors received the offer for Mia’s heart until the two surgeries began concomitantly. The surgeries began around 7 p.m. Wednesday evening, with Mia and Brooklyn in operating rooms across the hall from each other.
“We went into the operating room at the same time and our donor team told me that the donor heart was good. Once I knew they were on their way back [with the heart], I made the incision [in Mia’s chest],” says Dr. Goldstone. “Dr. Kalfa had already made an incision in Brooklyn once we had accepted the heart so that he would be in the right timeframe for needing the valves too. I then proceeded with the heart transplant.”
After performing a sternotomy, Dr. Goldstone explanted Mia’s heart, which was transferred to Dr. Kalfa in the operating room across the hall. He then continued with implanting the donor heart in her chest Already having performed Brooklyn’s sternotomy in preparation to receive the donor valves, Dr. Kalfa took Mia’s explanted heart and harvested the aortic and pulmonary valves and roots – first the pulmonary and then the aortic – and then ligated the coronary arteries in the explanted heart. Then he implanted the aortic root in the truncus position, detached the coronary arteries from the old aorta and re-implanted them into the new living allogeneic aortic root. “Each allogeneic root was trimmed and prepared in a way to fit the anatomy of Brooklyn’s heart,” says Dr. Kalfa. “That’s a pretty complex operation on a baby like Brooklyn, who already had a previous operation.”
Drs. Bacha and Kalfa preparing the new valves for Brooklyn during the partial heart transplant
Brooklyn’s operation took approximately 10 hours and Mia’s took approximately six. Both patients were weaned off cardiopulmonary bypass with stable hemodynamics and had normal EKGs before their chests were closed without impact.
Recovery and Implications for the Future
Mia’s heart transplant and Brooklyn’s partial heart transplant went smoothly. Both patients have since been discharged and continue to have an uncomplicated postoperative course. “Infants typically do extremely well after transplant,” says Dr. Richmond. “We expect [Mia] to meet all the normal baby milestones and then very quickly, all the toddler and preschool things that we would ever want her to do. She has very few, if any, limitations on her lifestyle moving forward…Brooklyn’s heart function is already improving from what it was before the operation. Both valves are functioning beautifully without any concerns…We expect her to recover and thrive and grow and do all the normal things that we would want her to do.”
Front row (left to right): Mia and Brooklyn with their parents following discharge from the hospital after the domino partial heart transplant.
Back row (left to right): NewYork-Presbyterian/
For the doctors, this is one case that they will never forget. “Anytime you do something for the first time, you go into that new endeavor understanding the risks and understanding the impact it may have on the families and children you care for,” says Dr. Richmond. “Seeing how quickly both of these infants recovered and seeing how grateful the families are motivates us to continue to push the envelope, continue to offer these newer techniques.”
“To be a part of this really makes you so excited,” says Dr. Goldstone. “Day-to-day, this job can be stressful, but something like this completely rejuvenates you and reinforces why I became a doctor.”
The success of the domino partial heart transplant at NewYork-Presbyterian/
The NewYork-Presbyterian/
To help broaden the use of living allogeneic partial heart transplants, Dr. Kalfa says that he’s been in touch with others who have performed these surgeries to discuss the cases and learn from each other. “We are thinking about creating a consortium and a registry to collect all the data from these patients receiving this new procedure nationwide,” he says. “Locally, we are now working on organizing our partial heart transplant program in a systematic way to streamline the identification of donors and recipients so that this new procedure can benefit the maximum number of children and have the highest impact on their lives.”
Dr. Kalfa adds that the expertise and multidisciplinary collaboration found at NewYork-Presbyterian/