NICU Clinical Integration System Takes Patient Safety to the Next Level
The new clinical integration system at New York-Presbyterian/Weill Cornell Medical Center’s level IV neonatal intensive care unit (NICU) is ringing all the right alarms. Born out a need to effectively communicate with NICU nurses and doctors in the new architectural layout of NewYork-Presbyterian Alexandra Cohen Hospital for Women and Newborns, the integration system is helping to increase patient safety and reduce NICU-related parental stress and anxiety.
“The ability to know in real-time what is happening really helps to optimize resuscitation, organize people better, and helps parents feel reassured. Our NICU response time is so fast—within seconds, which is really incredible,” says Catherine L. Chang, MD, a neonatologist at New York-Presbyterian/Weill Cornell who is the lead physician helping to implement the user-driven clinical integration system.
“Our NICU response time is so fast. People respond within seconds, which is really incredible.” — Dr. Catherine Chang
Moving the NICU from an 11,000 square foot unit with 5 rooms of about 10 babies to a 44,000 square foot NICU with 51 private, single-family rooms was no small feat. The new space supports the hospital's mission to practice family-centered care. Still, infants' geographic spread in the NICU presented a unique challenge and placed significant stress on nursing staff, who each typically care for 2 to 3 babies and must respond in seconds during an emergency.
Optimizing Patient Safety
“We had to extend our reach somehow,” says Dr. Chang who was tasked, alongside Jeffrey M. Perlman, MB, ChB, Chief of Neonatology at New York-Presbyterian/Weill Cornell, with ensuring patient safety in the new NICU. “It was a collaborative effort involving nursing leadership, NICU clinical managers, information technology experts, medical providers, and hospital administrators. We utilized technology to do the legwork for us,” says Dr. Chang.
“This is a superb patient safety system. You hit a button and many providers respond rapidly to a designated, targeted area.” — Dr. Jeffrey Perlman
“Other centers with single bed NICU’s have clinical integration systems, but what makes NewYork-Presbyterian unique is how we integrate the technology into all of our other platforms and how this provides multiple layers of protection and safety for each patient. We built this system with nurses, nurse practitioners, physician’s assistants, respiratory therapists, and providers in mind,” explains Dr. Chang.
“If there is a baby with impending cardiac arrest, the entire unit gets an alert, including the resuscitation team, with the name and geographic location. What is unique is that we also utilize Vocera—a push-to-talk device—where we can automatically speak to everyone on the resuscitation team,” says Dr. Chang who is Director of Resuscitation and Simulation at New York-Presbyterian/Weill Cornell’s NICU.
Vocera’s push-to-talk device acts like a walkie talkie, allowing NICU nurses and providers to communicate with each other when a baby needs immediate medical attention. The first provider to arrive can initiate an intervention (such as positive pressure ventilation or chest compressions) while simultaneously providing critical information over Vocera to other providers as they are running to the call.
“We know that the more information the team has before they arrive, the better. In emergency situations, when every second counts and team members are running from different locations, having a shared mental model early on improves team cohesion and performance—ensuring an optimal resuscitation,” says Dr. Chang.
Simulation Training
In a typical open-bay NICU, there are multiple babies and nurses in the same room. To transition staff to a system where they had to keep tabs on multiple babies, each in different rooms, Dr. Chang led education and simulation training for nurses and providers—helping to pilot the new system.
“In an open-bay layout, cross-monitoring and situational awareness occurs more easily,” says Dr. Chang describing the previous unit. “Even if a nurse was not assigned to a patient, they know what’s happening and how to intervene because they have been in the same room all day with them,” explains Dr. Chang.
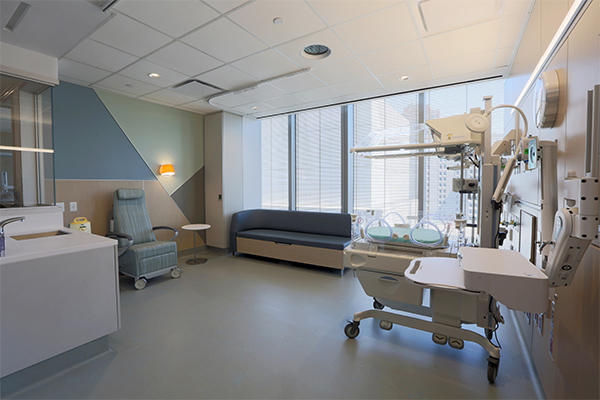
Private, single-family NICU rooms at NewYork-Presbyterian Alexandra Cohen Hospital for Women and Newborns are designed to accommodate singles and twins—all with our state-of-the-art clinical integration system to optimize patient safety.
In the new private single-family NICU layout, the primary assigned nurse is situated in an alcove right outside each of the 51 private rooms (42-single and 9-twin rooms) where he/she can directly visualize 2 monitors. Heart rate, respiratory rate, oxygen saturation, and blood pressure readings are visible on the cardiopulmonary monitor system available to nurses and parents alike.
Since implementing the new clinical integration system in August 2020, Dr. Chang’s team is on their 5th iteration, fine-tuning the system to incorporate feedback from nurses and families. Input from nursing leadership has been invaluable to moving the initiative forward.
“The nurses are on the frontline. We meet each month to talk about changes in terms of how we arrange zones or timing in our layers of safety. There is a balance between alarm fatigue and patient safety, which is critical in terms of implementation,” says Dr. Chang.
NICU-Related Parental Stress
The emotional distress and anxiety that comes with having a baby in the NICU can take a toll on parents. The new single-family rooms and the clinical integration system at New York-Presbyterian/Weill Cornell are helping to reduce NICU-related parental stress, increase skin-to-skin contact, increase parental involvement, and ultimately giving parents more confidence in caring for their preterm/critically-ill infant once they return home.
“It is the best balance for parents to be able to have one-on-one time with their baby, but at the same time have an alert system where they know a whole zone of nurses are always watching. The technology in the clinical integration system reassures parents that their baby is safe, which often alleviates anxiety.” — Dr. Catherine Chang
The 51 family rooms—including 9 larger rooms that accommodate twin babies— have been getting rave reviews from families and include a sink, locker, personal breast pump, recliner, pullout bed, and a view. “Parents love the space and once they see how the clinical integration system works, they really start relaxing and enjoying the beautiful room with their baby,” says Dr. Chang.
Constantly Improving
Implementing such a complex system, required the ability to innovate and pivot quickly. “We had to be able to go to IT in real-time and turn on a dime to keep babies safe and help parents stay as sane as possible. This is someone’s baby—their most precious family member—and we take that responsibility extremely seriously,” says Dr. Chang.
Related Publications