A CT scan, or computed tomography scan, is a diagnostic imaging procedure that combines a series of X-ray images taken from different angles around the body to create detailed cross-sectional images, or slices, of the body's internal structures. These images can be more detailed than conventional X-rays, making CT scans particularly useful for diagnosing a wide range of conditions. They are very effective in detecting traumatic injuries such as fractures, internal bleeding, or organ damage resulting from accidents or falls.
The mnemonic used by Dr. Andrew Perron who lectures on this topic frequently is: "Blood Can Be Very Bad". Content and images below are taken from his lecture (with his permission).
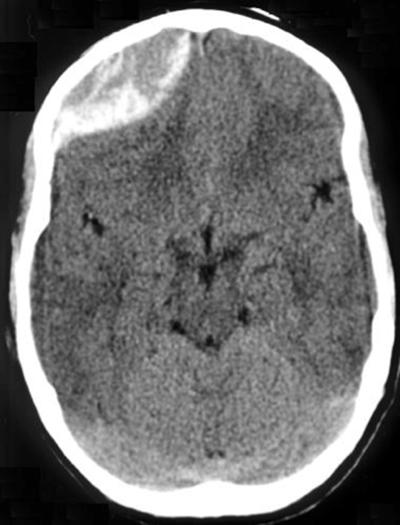
Step 1: Blood
BloodThe first step in reading a head CT scan is looking for any evidence of bleeding throughout all slices of the head CT.
Blood will appear bright white and is typically in the range of 50-100 Houndsfield units.
Basic categories of blood in the brain are epidural, subdural, intraparenchymal/intracerebral, intraventricular, and subarachnoid.
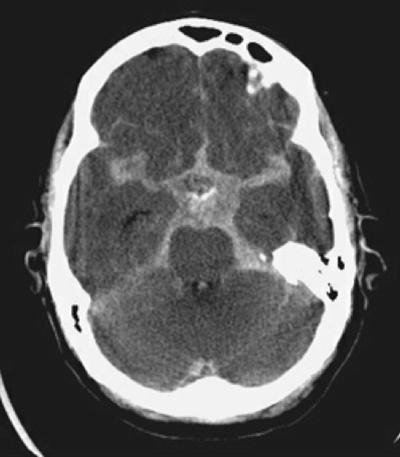
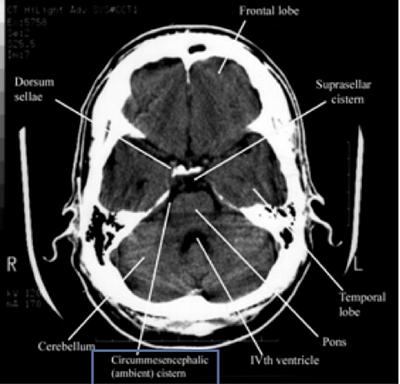
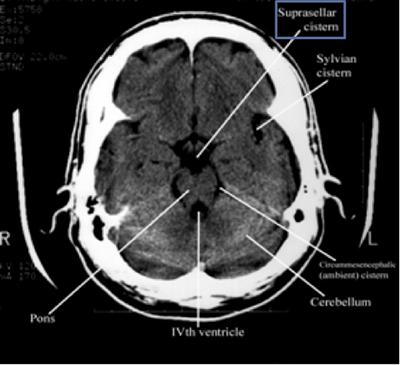
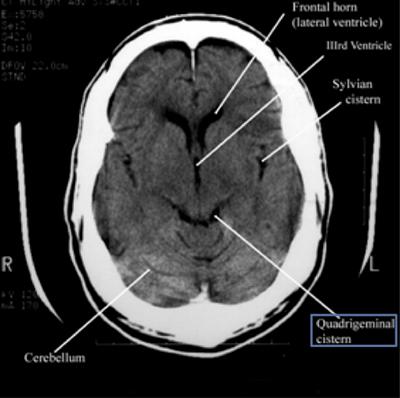
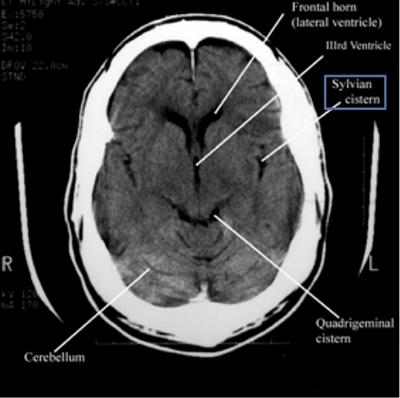
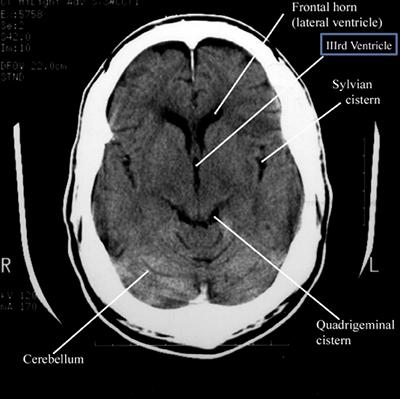
Step 2: Cisterns
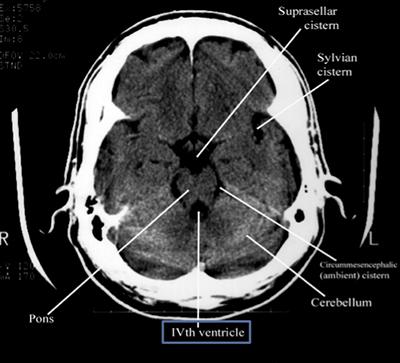
CisternsCisterns are the compartments within any of the openings in the subarachnoid space of the brain filled with cerebrospinal fluid. Two key questions to answer regarding the four key cisterns (Circummesencephalic, Suprasellar, Quadrigeminal and Sylvian)
- Is there blood?
- Are the cisterns open?
Step 3: Brain
BrainExamine the brain for:
- Symmetry - make sure sulci and gyri appear the same on both sides. (easiest when patient not rotated in the scanner)
- Grey-white differentiation - the earliest sign of a CVA on CT scan is the loss of the grey-white interface on CT scan. Compare side to side.
- Shift - the falx should be in the midline with ventricles the same on both sides. Check for effacement of sulci (unilateral or bilateral).
- Hyper/hypodenisty - blood, calcification and IV contrast are hyperdense (appear lighter) and air, fat and areas of tumor ischemia are hypodense (appear darker).
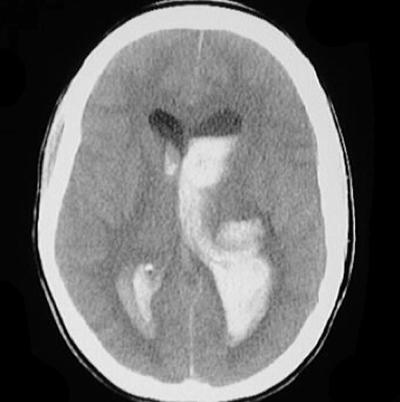
Step 4: Ventricles
VentriclesExamine for IIIrd, IVth and lateral ventricles for dilation or compression/shift.
Pathologic processes cause dilation (hydrocephalus) or compression/shift. Communicating vs. Non-communicating. Communicating hydrocephalus is first evident in dilation of the temporal horns (normally small, slit-like). The lateral, IIIrd, and IVth ventricles need to be examined for effacement, shift, and blood.
Step 5: Bone
BoneBone has the highest density on CT scan (whitest in appearance.) Evaluate for fracture.
See More Medical Resources at NewYork-Presbyterian
See More ResourcesContent Block: NewYork-Presbyterian provides educational information about medical topics. You can find these resources at NewYork-Presbyterian Neurology and Neurosurgery.