Promoting Global Lung Health

Dr. Neil W. Schluger
Tuberculosis, asthma, HIV, and chronic obstructive pulmonary disease plague developing countries around the world. Among the many healthcare challenges they face are limited medical resources and very few pulmonary physicians to provide basic services at the primary and secondary care level. Following are some of the transformative efforts underway by NewYork-Presbyterian/Columbia University Medical Center physicians to bring expertise in pulmonary medicine to countries in dire need of such specialized care.
Building and Growing a Model Training Program
With a population of over 100 million people, Ethiopia is one of the largest countries in Africa, but also one of the poorest. It has fewer physicians per capita than almost any country in the world. It also has high rates of tuberculosis and acute respiratory infections and a significant burden of chronic obstructive lung disease and asthma. And yet in 2011, the country had virtually no practicing pulmonary physicians. That is until the situation came to the attention of Neil W. Schluger, MD, Chief of Pulmonary and Critical Care Medicine at NewYork-Presbyterian/Columbia.
“The Ethiopia project started with a call I got out of the blue from someone I had never met who was working here at NewYork-Presbyterian,” says Dr. Schluger. “She was well connected in Ethiopia through the Addis Ababa University School of Medicine. They were seeking help in developing training programs for doctors and she was led to me.”
Soon after Dr. Schluger met with a physician from the Ethiopian medical school who came to New York and explained their vast needs. Dr. Schluger then took on what he calls the “interesting challenge of picking a big country with no lung doctors to see if we could train some lung doctors!”
In 2012 Dr. Schluger traveled to Addis Ababa with a colleague from Brown University who had previously worked in Kenya. “We got to know the head of the medical school, the dean, the chief executive, and the director, as well as the Ministry of Health for Ethiopia. Then we said, ‘Okay, in 2012 we’re going to start a fellowship program in Ethiopia and train physicians to be pulmonary doctors in Ethiopia.’ It was a handshake deal. We returned to New York and realized that we had committed ourselves to something starting in a year and we had nothing!”
Supported by the World Lung Foundation, the East African Training Initiative (EATI) was born, with a commitment to begin fellowship training in 2013. “I spent a lot of 2012 in preparation and any pulmonary doctor that I knew in the U.S. who was unlucky enough to sit next to me in a meeting got a recruiting pitch,” recalls Dr. Schluger.
The next order of business was to write the curriculum. “Our aspiration was to do this on a very high level,” says Dr. Schluger. “We didn’t want a program where American doctors would show up a couple of times a year, give a few lectures, and leave. We also wanted to have someone on the ground in Ethiopia nearly full-time. We felt that a continual presence was necessary to achieve a high level of competence, as well as to exemplify and instill a culture of professionalism in trainees. It would have to be a real program modeled very closely on what we would do for physicians in the best American programs at leading academic medical centers. So, we designed a curriculum that was very much derived from how we train our pulmonary fellows here at Columbia.”
It turned out that faculty recruitment was no problem. “There were a number of people who were very interested; some had worked in Africa and some had not. Dr. Charles Sherman, another colleague from Brown, also devoted a tremendous amount of time to the recruitment effort.
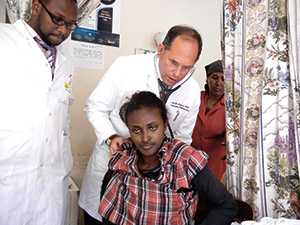
“We launched the program in January 2013, and today we have a total of 45 faculty who have volunteered. We also have someone in Addis about 40 weeks a year,” continues Dr. Schluger. “Our core of very dedicated faculty go frequently and find it very rewarding.”
The two-year program to date has trained three classes of fellows. The fellows undergo a rigorous program of pulmonary medicine, with content specifically tailored to local hospitals and the population. “We have seven well-trained pulmonary doctors and six more who are currently in training,” says Dr. Schluger. “We feel very good about the people we’ve trained. They meet a high standard of knowledge and practice in pulmonary medicine. We examine them rigorously with written and bedside exams. They also move very quickly into leadership positions in Ethiopia.”
Today EATI is the only training program in pulmonary medicine anywhere in sub-Saharan Africa outside of South Africa. It is supported by Vital Strategies, a global health organization for which Dr. Schluger serves as Science and Education Advisor, and the Swiss Lung Foundation.
As the program has flourished, so has the intent to increase a greater presence throughout the country. “Our graduates have started the Ethiopian Thoracic Society and conduct a continuing education meeting every year attended by 100 or so people,” says Dr. Schluger. “Attendees learn about major issues in lung health. And the Ministry of Health now has a group of doctors with expertise in lung disease that it can go to.”
Dr. Schluger offers high praise for the physicians in Ethiopia. “The talent pool is very large and the physicians are smart, hardworking, and ambitious. That is incredibly gratifying,” he says. “We do have a commitment in our division to continue. The people in Ethiopia are also interested in starting training programs in other specialties, and I believe we have created a model that they can follow. We see the world as a very interconnected place, and that is why these kinds of activities are so important.”
Stemming the Spread of Infectious Diseases

Dr. Max R. O'Donnell
For more than two decades Max R. O’Donnell, MD, MPH, has been at the forefront of efforts to end the epidemic of infectious diseases here and abroad. Dr. O’Donnell, a pulmonologist in the Division of Pulmonary and Critical Care Medicine at Columbia, devotes much of his time to research in TB, HIV, and global health, particularly in Africa.
“Drug-resistant tuberculosis is an important global public health concern because of its increasing incidence, low cure rates, and high mortality,” says Dr. O’Donnell, who first confronted the disease in Ethiopia in a rural community in 1995. “I was working on TB and HIV and this was before antiretroviral therapy. There were a lot of very poor outcomes, and we realized that tuberculosis was the leading edge of the HIV epidemic in Africa. That’s what really drew me into pulmonology as a field. Historically, pulmonary medicine has been involved in tuberculosis and respiratory infections, although a lot of people that work in the field currently are infectious diseases doctors.”
According to Dr. O’Donnell, nowhere has the increased incidence of TB and HIV generated more concern than in South Africa, where interactions between TB and generalized HIV/AIDS outbreaks are causing explosive increases in TB incidence and TB case-fatality rates. The most drug-resistant form of tuberculosis — extensively drug-resistant tuberculosis (XDR-TB) — is increasingly prevalent here.
“Our goal is twofold — to discover new infectious diseases as they emerge into the population and to discover diseases that are vaccine-preventable.”
— Dr. Max R. O’Donnell
In addition, Dr. O’Donnell, who is also an Assistant Professor of Medicine and Epidemiology at Columbia University Medical Center, serves as a research associate at the Centre for AIDS Programme of Research in South Africa (CAPRISA). “Much of my work is centered in South Africa, but I also work in Ethiopia and Uganda. My efforts in TB involve both the lab, as well as enrolling patients in drug-resistant TB and HIV studies,” says Dr. O’Donnell, who collaborates closely with Ian Lipkin, MD, an internationally recognized epidemiologist at Columbia University Mailman School of Public Health. “We’re using new and exciting assays developed by the Lipkin lab to try to understand lung viral infections and other emerging infectious diseases. We have a major study underway with about 9,900 adults and children in Uganda looking at causes of unknown presentation with severe, acute respiratory infection.”
Uganda, notes Dr. O’Donnell, “is an emerging infectious diseases hot spot. The human population living near forests and jungles is just part of the story. Another major issue is the peri-urban slums where you might find up to 10 people living together in a shack with limited access to water or sanitation. It’s that permissive type of environment where viruses can spread.”
Dr. O’Donnell and his team are working with the Uganda Virus Research Institute in Entebbe, which has established a national network of surveillance sites. “Dr. Matt Cummings, a pulmonary critical care fellow at Columbia, is gathering samples that will be shipped to the lab here, where we will use a new assay that Dr. Lipkin’s group has developed,” says Dr. O’Donnell. “Our goal is twofold — to discover new infectious diseases as they emerge into the population and to discover diseases that are vaccine-preventable. For example, an outbreak of severe measles and pneumonia in Uganda is something we can address. We need to do better with vaccinations and prevention. People in this day and age don’t need to die of measles and pneumonia. This sort of precision surveillance will help us figure out when there are new, emergent diseases and whether they are outbreaks of vaccine-preventable disease.”
Dr. O’Donnell and Dr. Neil Schluger have also launched a new four-year fellowship program at Columbia — the Global Health Research Pathway — that focuses on global lung health using basic, clinical/translational, policy, and implementation science approaches.
“Global health does not exist in isolation,” says Dr. O’Donnell. “When you get down to the molecular level you start to track disease and, lo and behold, people are bringing disease into Africa as well. For example, we identify a strain in London and then it pops up in Uganda or wherever. It’s worth thinking about. Even if we feel like we want to be isolated from everyone else, we’re not.”
“From a population basis, we need to draw on genomics to think about vulnerable populations and use big data and spatial modeling to figure out spots where diseases emerge and then direct the right resources to them,” he adds. “One-size-fits-all public health solutions are just as obsolete as one-size-fits-all chemotherapy. In the next 10 to 15 years people are going to start to think about global health this way. That, to me, is going to be very exciting. We need to use science and resources to advance an agenda that will improve the health of people around the world. It’s pretty ambitious, but we have a lot of talented people working on it.”
Reference Articles
Padayatchi N, Naidu N, Friedland G, Naidoo K, Conradie F, Naidoo K, O’Donnell MR. Turning the tide against tuberculosis. International Journal of Infectious Diseases. 2017 Mar;56:6-9.
Sherman CB, Carter EJ, Braendli O, Getaneh A, Schluger NW. The East African Training Initiative. A model training program in pulmonary and critical care medicine for low-income countries. Annals of the American Thoracic Society. 2016 Apr;13(4):451-55.
Cummings MJ, Bakamutumaho B, Kayiwa J, Byaruhanga T, Owor N, Namagambo B, Wolf A, Wamala JF, Morse SS, Lutwama JJ, O’Donnell MR. Epidemiologic and spatiotemporal charac-terization of influenza and severe acute respiratory infection in Uganda, 2010-2015. Annals of the American Thoracic Society. 2016 Dec;13(12):2159-168.
O’Donnell MR, Padayatchi N, Kvasnovsky C, Werner L, Master I, Horsburgh CR Jr. Treatment outcomes for extensively drug-resistant tuberculosis and HIV co-infection. Emerging Infectious Diseases. 2013 Mar;19(3):416-24.
Related Publications

East African Training Initiative at Work in Ethiopia





