Among patients with congenital heart disease, particularly those who have undergone single ventricle palliation, there is a subset of patients who will develop lymphatic abnormalities. These potentially serious complications, which include chylothorax, plastic bronchitis, and protein-losing enteropathy, can be quite debilitating and difficult to manage medically. However, in the last several years, the availability of new treatment techniques and advances in modalities for lymphatic imaging have made it possible to offer interventions that can be life changing, significantly improving quality of life and reducing the morbidity and mortality associated with these conditions..
At NewYork-Presbyterian Morgan Stanley Children’s Hospital, Michael P. DiLorenzo, MD, is a pediatric cardiologist specializing in noninvasive imaging, including echocardiography, cardiac MRI, and CT, and is Co-Director of the Pediatric Comprehensive Marfan Clinic; Matthew A. Crystal, MD, is a pediatric interventional cardiologist and the Director of Inpatient Cardiology; and Sheryl Tulin-Silver, MD, is Director of Pediatric Interventional Radiology and Co-Director of the multidisciplinary Vascular Anomalies Group. Having already collaborated in the care of patients with varying manifestations of congenital heart disease, Drs. DiLorenzo, Crystal, and Tulin-Silver saw another opportunity to combine their expertise and experience to elevate treatment for children presenting with lymphatic disorders with a goal to decrease hospital and ICU length of stay overall and reduce frequent readmissions for patients with plastic bronchitis and protein-losing enteropathy.

Dr. Michael DiLorenzo

Dr. Matthew Crystal

Dr. Sheryl Tulin-Silver
“We came together to develop a comprehensive lymphatic imaging and intervention group encompassing a large multidisciplinary effort to provide contrast-enhanced MR lymphangiography and percutaneous lymphatic interventions for patients with congenital heart disease. Subsequently, we plan to expand the program to outpatients and patients with non-cardiac lymphatic disorders,” says Dr. DiLorenzo, Assistant Professor of Pediatrics at Columbia. “There are very few centers in the country providing dedicated services for this population on a large scale. Working with NewYork-Presbyterian’s Congenital Heart Center, which has one of the highest volume programs in the country, we realized that we could provide an important service to our patients with congenital heart disease and to families throughout the New York region and Northeast who might not have access to this level of complex care.”
“Having a longstanding, high volume congenital heart program that cares for patients ranging from the prenatal period through late adulthood engenders a very close-knit collaborative environment involving cardiac specialists in imaging, catheterization, surgery, anesthesiology, intensive care for newborns and children, as well as an interventional radiologist and a phenomenal, allied health team,” notes Dr. Crystal, Associate Professor of Pediatrics at Columbia. “Our new procedural pathway for lymphatic disorders brings everyone together in a way that is not typically done. And our collective expertise in our respective fields positions us to optimize outcomes for patients who have a rare condition and a rare complication of that rare condition.”

Multidisciplinary Lymphatics Intervention Program at NewYork-Presbyterian Morgan Stanley Children’s Hospital
Orchestrating Precision Imaging and Immediate Intervention
“There are a number of ways that we can image the lymphatic system, including techniques not involving contrast,” explains Dr. DiLorenzo. “But without contrast, you do not obtain the fine detail of the lymphatic system that a good contrast image will provide. This is where a multidisciplinary team is necessary. Each procedure is labor intensive, involving some 20 people with an all-hands-on deck approach to make sure we can obtain the images we need. This includes a high level of coordination between the fluoroscopy suite, the MRI suite, and the catheterization/
“In particular, positioning the patient during these imaging and interventional procedures is critical,” adds Dr. Tulin-Silver, Assistant Professor of Radiology at Columbia. “The patient needs to be on an MRI-compatible and radiolucent transfer board, which we pad to avoid pressure on the joints. This enables us to easily transport the patient between the fluoroscopy suite and the MRI suite. In addition, all of the physiological monitors need to be changed prior to transferring the patient from the fluoroscopy suite to the MRI room. Every little detail needs to be perfectly coordinated among 15 to 20 people.”
In the fluoroscopy suite, Dr. Tulin-Silver places small needles into the patient’s inguinal lymph nodes at the top of the leg and glues them in place so they do not dislodge during transfer of the patient to the MRI suite. “Sometimes, the lymph nodes can be several millimeters in size. So it’s a very precise process placing the needles,” she says. When placing the needles, Dr. Tulin-Silver uses ultrasound guidance and fluoroscopic confirmation with radiopaque contrast material.
In the MRI suite, Dr. DiLorenzo performs thoracic lymphatic MRI imaging with and without gadolinium-based contrast injection. Dr. Tulin-Silver is positioned inside the MRI room with the patient, injecting the contrast very slowly. “The importance of administering the contrast is that we are actually watching the flow within the lymph nodes in real time, essentially viewing a video map,” she explains. “We inject the contrast into the lymph nodes at the top of the leg and we track its course with multiple MRI scans every few seconds. By following the stepwise movement of the contrast, we are able to identify small areas of leak, anatomical variations, or blockages and other concerns of that nature that are best appreciated with real-time MRI images.”
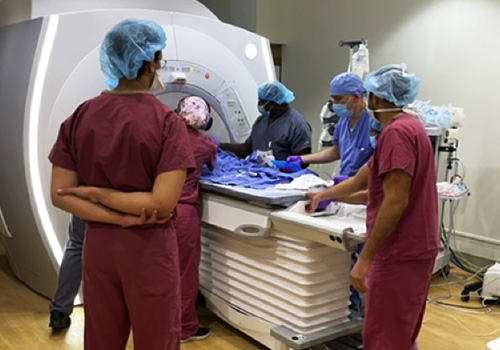
Members of the team prepare for MRI lymphatic imaging.
“These MRI images can be manipulated in all directions,” adds Dr. DiLorenzo. “You can look at multiple views from any angle so that you can see where the abnormality is in relation to other structures.”
“What is important to recognize is that while the MRI and contrast injection is not that dissimilar in theory and in principle to a patient having an intravenous line placed for injecting contrast to observe the flow of blood, the distinction is in Dr. Tulin-Silver’s expertise in obtaining access to a lymph node, which cannot be achieved with an IV injection,” says Dr. Crystal. “The process is done by hand and the flow of contrast is slower. So the success of the approach for imaging lymphatic abnormalities is predicated on the expertise of Dr. Tulin-Silver in accessing lymph nodes and Dr. DiLorenzo’s skill in obtaining the images.”
“In several of our recent cases, findings from the images that we obtained changed our management plan,” says Dr. Tulin-Silver. “They very clearly indicated a fork in the road that helped direct treatment after collaboratively reviewing the images and incorporating them into the overall clinical picture. The technical success related to the information we learn through the MR imaging translates into a clinical success with excellent patient outcomes.”
“We all review these images together and if an intervention is deemed suitable, the patient is transferred from the MRI suite to the interventional/catheterization suite where Dr. Tulin-Silver and I work together,” says Dr. Crystal. “The MRI imaging can be merged with the images obtained in the fluoroscopy suite to help guide our access and targets for the procedure. We will use MRI image guidance and lymph node injection with Lipiodol to direct thoracic duct access and, depending on the specific lymphatic abnormality, thoracic duct embolization will be performed by glue or coil embolization.”
“Not all children who present with a lymphatic abnormality will require an intervention,” continues Dr. Crystal. “Generally, patients with severe congenital heart defects such as tetralogy of Fallot and single ventricular heart disease are more prone to lymphatic complications needing an intervention. At our center, chylous effusions are of particular interest to our surgical team and congenital heart malformations team.”
“Patients with chylothorax that does not resolve spontaneously are typically managed with chest tubes for pleural drainage, a severely fat-restricted diet, total parenteral nutrition, or IV infusions of octreotide. If these approaches are unsuccessful, we are able to perform an intervention to either resolve a stenosis or address channels that need to be embolized,” adds Dr. Tulin-Silver.
Following the interventions, patients are admitted to the ICU for 24 to 48 hours for hemodynamic management of post-procedure capillary leak and treatment with broad-spectrum antibiotics.
“What is very special about our lymphatics program are the relationships that we all have with each other, the respect that all of us have for each member of our team, and how well we work together to manage these complex patients,” says Dr. Tulin-Silver. “This is the foundation of our success and will enable us to realize our goal of becoming a regional center of excellence and innovation in lymphatic imaging and percutaneous interventions.”



