What began as a concern a number of years ago about a surgical complication observed by Michael G. Vitale, MD, inspired a transformational initiative in spine deformity surgery safety that is today unparalleled. In 2014, Dr. Vitale and colleagues in the field launched The Safety in Spine Surgery Project (S3P) to improve the safety of surgical treatment of spine problems in adult and pediatric populations by developing best practice guidelines at its foundation.

Dr. Michael Vitale
“This initiative is about how we can collectively make spine surgery safer together,” says Dr. Vitale, who is Chief of Pediatric Spine and Scoliosis Surgery in the Department of Orthopedic Surgery at NewYork-Presbyterian/Columbia University Irving Medical Center. He also serves as Vice Chair, Quality and Strategy, Orthopedic Surgery, and the Ana Lucia Professor of Pediatric Orthopedic Surgery and Neurosurgery at Columbia. “Key to this goal was the establishment of an annual spine safety summit. For a number of years, we held the program in New York with standing room only. The meeting sold out six years in a row. In the last few years, we began simulcasting the program because the demand was so high.”
“During the last two years, S3P offered virtual webinars, and importantly with regard to scale of messaging, the leadership mobilized a very large social media awareness effort,” adds Dr. Vitale. “Last year, there were 225,000 engagements around this concept of safety in spine surgery with all the major organizations – Scoliosis Research Society, Pediatric Orthopedic Surgery of North America, and study groups – jumping on board and helping to boost that messaging.”
Every year, the meeting focuses on developing a best practice guideline for a specific area in spine surgery, ranging from how to avoid wrong site surgery, responding after loss of intraoperative neuromonitoring signals in the operating room, implementing halo-gravity traction, and preventing infection, as well as those addressing particular issues in complex spine deformity surgery. This is accomplished through expert panels and a formally derived consensus process, the Delphi process. The resulting guidelines have led to some of the most widely cited publications in this field.
As spine surgeons, we have a broader obligation to patient safety that leverages each of our skills, perspectives, and knowledge to create best practice guidelines and then promulgate them through education.
— Dr. Michael Vitale
“These panels are comprised of thought leaders who are deeply committed and have carefully considered how to make spine surgery safer,” says Dr. Vitale. “They are a group of people representing not only the spinal deformity space, but also cervical spine, degenerative disease, and adult and pediatric minimally invasive surgery, and we continue to broaden our audience around different areas in spine surgery. When we get together, we share methods we are doing differently and come up with a product that's better than the sum of its parts.”
Recent Studies Address Neurological Events and Surgical Site Infections
During the past year, Dr. Vitale, his colleagues at Columbia, and members of S3P and other specially convened expert panels have continued developing best practice guidelines on a number of critical safety issues that continue to confront spine surgeons. Their efforts provide the surgical team with resources that can help drive decisions in unexpected events and optimally preserve the neurological function of patients and curtail the incidence of surgical spine infections.
Neurological Events
In 2014, Dr. Vitale and his colleagues on the S3P expert panel developed the organization’s first formal guidelines, which targeted responding to intraoperative neuromonitoring changes in the operating room. The resulting paper, published in the September 2014 issue of Spine Deformity, was the most widely cited paper in the field. These guidelines have just been expanded upon by Dr. Vitale, Lawrence G. Lenke, MD, Surgeon-in-Chief and Co-Director of Och Spine at NewYork-Presbyterian, and 13 other experienced spinal deformity surgeons across the country. The study team further developed the original consensus-based best practice guidelines to optimize the approach to intraoperative neuromonitoring events associated with “high-risk” spinal deformity surgery. This set of guidelines, published in the July 2022 issue of Spine Deformity, included a response algorithm; ongoing considerations of etiology – systemic, destabilization/
In a companion paper, published in the same issue of Spine Deformity, the expert panel focused on parameters that constitute elevated risk during spinal deformity surgery and potential preventative strategies that may minimize the risk of intraoperative neuromonitoring events and postoperative neurological deficits. The panel identified and achieved consensus on 22 determinants of high-risk items, incorporating 8 patient factors, 8 curve and spinal cord factors, and 6 surgical factors, as well as 21 preoperative (4), intraoperative (14) and postoperative (3) preventative strategies.
Surgical Site Infections
Faced with surgical site infections (SSI) that continue to prevail even with numerous measures developed and implemented to reduce their incidence, Dr. Vitale, Dr. Lenke, along with their Columbia colleagues in the Department of Orthopedic Surgery and at six other major orthopedic centers across the country, came together to develop a prediction model that could quantify the risk of SSI for individual pediatric spinal deformity patients.
Their study included 3,092 spinal deformity surgeries of which there were 132 cases (4.3 percent) of SSI. The final prediction model contained 9 variables based on their ability to predict SSI within 90 days postoperatively:
Patient Characteristics
- Overweight or obese body mass index (BMI)
- Neuromuscular etiology
- American Society of Anesthesiologists (ASA) grade >2
- Non-ambulatory status
- Abnormal hemoglobin level
Surgical Factors
- Revision surgery
- Pelvic instrumentation procedure
- Procedure time ≥7 hours
Hospital Factor
- <100 spine surgical cases per year per institution
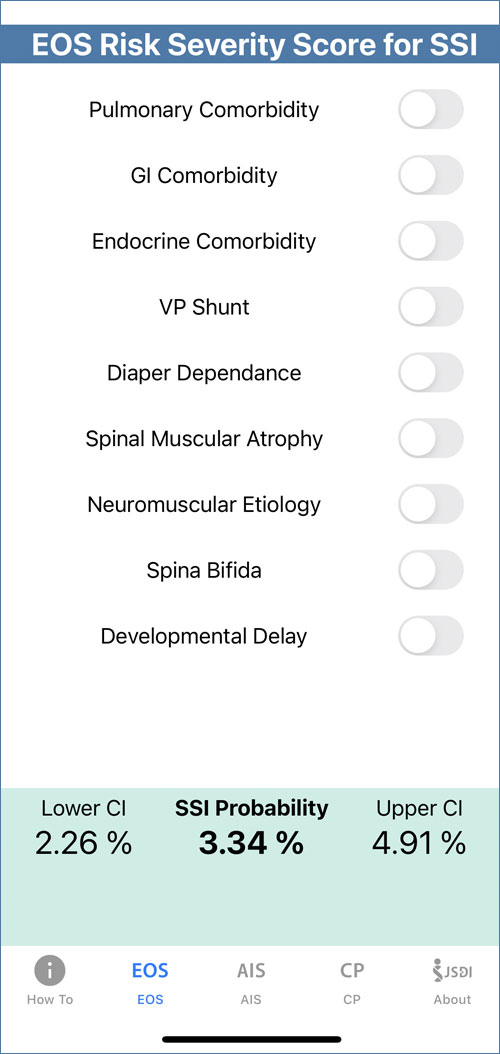
Surgical Site Infection Risk Severity Score Calculator based on research by Columbia Orthopedics and the Children’s Spine Study Group. The user-friendly graphical interface utilized in the smart phone application facilitates calculation of patient risk in clinical settings.
The authors note that the validated calculator enables the surgical team to identify high-risk patients, thereby providing the opportunity to address modifiable risk factors prior to surgery and increase vigilance of the particular surgical factors that increase the risk for SSI.
The Bigger Picture: Preventable Patient Harm
“The majority of complications we see are related to system failures,” notes Dr. Vitale. “I think we under-appreciate the reality that there is an entire episode of care that starts before surgeons enter the OR, whether it relates to skin prep or antibiotics, as examples, but also formal discussion about potential risks before the surgery. If you align your processes, you make it much less likely for the wrong problem to propagate through the system.”
“Approaching errors from the system-level perspective places greater emphasis on work conditions that result in human error and allows for countermeasures to be built into the organization to create a more effective work environment and workforce,” says Dr. Vitale in an article published in the May/June 2022 issue of the Journal of Pediatric Orthopaedics, which provides high-level recommendations for clinical and surgical practice. “Although safety in pediatric orthopedic surgery does depend on individual skill and expertise, it further requires a well-developed system approach.”
Dr. Vitale discusses how “a systems approach to health care delivery through the use of work-aids to aid clinical decision making, investing in one’s team and breaking hierarchies, and establishing a culture of psychological safety that can help address errors that result in preventable patient harm.”
Work-Aids: Checklists and guidelines can direct surgery, ensure that all evidence-based patient safety measures are complete, assist in task assignment, and formalize communication.
Team-Based Approach: Using a method such as the Comprehensive Unit-Based Safety Program (CUSP) can improve perioperative efficiency and promote a culture of safety. Engaging frontline staff members in quality efforts early on fosters greater investment in quality improvement and patient safety goals across the team.
Culture of Psychological Safety and Trust: Encouraging OR team members to voice their questions, concerns, or potential errors without the fear of reprisal inspires a mutual feeling of trust and respect that can improve team performance through improved communication and collaboration.
The systems-level approach is a strategy that Dr. Vitale and his colleagues have long applied to their own surgeries at NewYork-Presbyterian Morgan Stanley Children’s Hospital. “Because we are a very high volume facility with 350-plus pediatric spine surgeries a year, we have been able to create dedicated spine teams in which the same pediatric anesthesiologists are taking care of our patients and the same nurses who are in the operating room with us are also taking care of these patients in the clinic,” says Dr. Vitale. “We have a multidisciplinary preoperative indications conference prior to every case where we discuss patients with everyone who will be involved in their care.”
“The second key is that every aspect of the surgery and the surgical environment is highly standardized,” continues Dr. Vitale. “We have a standard set up for the OR table and for lights, as well as standard procedures for draping and prepping. And we have lots of checklists – for intraoperative neuromonitoring safety, for technical issues, and for parents. We also have formal data reporting mechanisms. I think every minute that you spend improving your processes by following best-practice guidelines and through structured communication with the team pays off with regard to better outcomes for patients.”




