The anticipated pain related to the immediate postoperative period following spine surgery is among the greatest concerns expressed by patients. At NewYork-Presbyterian/
“There are other issues and obstacles that patients have to deal with when they undergo spine surgery, but the acute experience of postoperative pain is often what they fear most,” says Dr. Joiner. “Fear of pain is one of the major barriers that patients must overcome before going ahead with any procedure to treat an issue with their spine – even if, ironically, surgery is ultimately necessary to relieve their chronic pain.”
In his own clinical practice, Dr. Mandigo, who has been performing spine surgery for more than two decades, sought to address the problem of pain control in the perioperative period by developing the x-ray-guided dorsal ramus block (XDRB), a local anesthetic injection that could be delivered by spine surgeons immediately prior to lumbosacral spine surgery.
“The goal of this block was two-fold,” says Dr. Joiner. “First, we want to reduce patient’s experience of postoperative pain. And second, if we can find other ways to manage postoperative pain, then we do not have to rely as much on opioid medications. Although surgeon-delivered blocks have been successfully used in joint replacement surgery and other non-spine orthopedic procedures, the use of nerve blocks within spine surgery remains less common.”

Dr. Evan Joiner
“Orthopedic subspecialists who focus on joints, for example—in collaboration with anesthesiologists—have done a great job of integrating nerve blocks into their practice, but the approach in spine surgery has only recently been explored,” continues Dr. Joiner. “While there have been a number of studies of ultrasound-guided nerve blocks for lumbar spine surgery,” he explains, “these types of spine blocks require a specialized anesthesiology to perform an additional procedure with additional equipment prior to surgery. What is unique to our neurosurgical spine practice at Columbia is that XDRB was developed within our own operating room workflow and existing protocols. We as spine surgeons are able to place our nerve blocks using the same x-ray equipment that we use to localize the operative level within the spine, which must be done for every spine surgery we do. This approach represents a seamless integration of a nerve block into our operative workflow. Furthermore, it complements our existing pain management strategies well, including multimodality pain medications such as Tylenol, gabapentin, muscle relaxants, and opioid medication.”
The radiography-guided bupivacaine injections target the dorsal rami of spinal nerves. “We insert a spinal needle just lateral to the midline, essentially where the transverse process meets the facet joint, and inject the bupivacaine into that region at multiple levels so that multiple levels of the spine are blocked,” explains Dr. Joiner. “This technique is adapted from outpatient pain management interventions such as facet joint blocks that are integral to conservative management strategies for lower back pain; however, they’ve never been used in the operating room in any formal way to reduce postoperative pain. The XDRB procedure, which takes an average of six minutes, is performed by the spine surgeon just before the incision.”
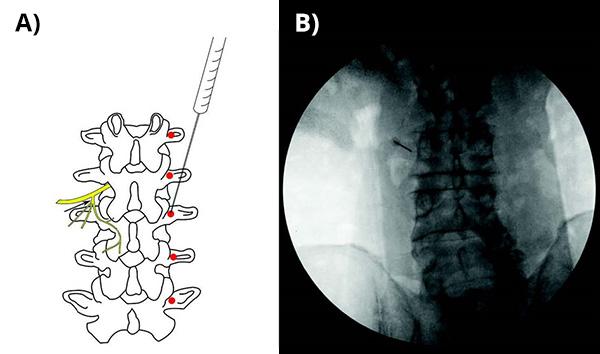
(A) An X-ray guided dorsal ramus block (XDRB) injection at junction of L3 superior facet and transverse process; lumbar nerve root is shown with ventral ramus and dorsal ramus (DR) and medial branch of DR.
(B) Intraoperative XDRB being placed at junction of left superior facet and transverse process at L3.
(Credit: JAMA Network Open, 2022 Dec 1)
Does XDRB Mitigate Postoperative Pain?
In theory, the concept of using a nerve block at the beginning of surgery would appear to have merit. To evaluate the benefit of XDRB, Dr. Joiner, Dr. Mandigo, and their neurosurgical colleagues at NewYork-Presbyterian/
While all the patients received total intravenous anesthesia, 58 them also underwent X-ray-guided bupivacaine injections targeted to the dorsal rami of spinal nerves, and the remaining 49 did not receive the injection.
“We used the visual analog pain score to characterize the patients’ level of pain in the post-operative period,” says Dr. Joiner. “The outcomes we recorded were the first pain score noted in the PACU when the patients were awake enough to respond to questions about their pain. We also tracked how much opioid medication the patients required while still in the PACU.”
The findings of the research team, which were published in the December 1, 2022, issue of JAMA Network Open, were encouraging. They included:
- Patients who received XDRB had mean first PACU VAS scores that were 1.5 points lower than those who did not have XDRB, representing a 39 percent reduction in pain scores between the two groups.
- Patients undergoing XDRB received 43 percent less opioid medication than those in the non-XDRB cohort.
“While this was a retrospective study, the results 40 percent lower pain scores and a 40 percent reduction on opioid use—there is very clearly an exciting signal here,” says Dr. Joiner. “XDRB shows promise for shifting the local anesthetic block from a distinct preoperative procedure performed by an anesthesiologist to an intraoperative surgeon-delivered procedure. Our findings have prompted us to now initiate a randomized control pilot study to further compare the use of nerve blocks versus no blocks in patients undergoing lumbar decompression or lumbar non-instrumented surgery. The pilot study will evaluate patients’ pain 24 to 48 hours beyond their PACU stay to determine their pain experience over time with the expectation that larger, fully powered randomized control trials will follow.”
“We believe that X-ray-guided nerve blocks have strong potential to become standard of care in spine surgery with relatively minimal changes in practice workflow,” adds Dr. Joiner. “The most compelling reason for pursuing this approach is to improve patients’ postoperative experience and reduce their pain and suffering.”




