In late 2023, Tomoaki Kato, M.D., chief of the Division of Abdominal Organ Transplant and Hepatobiliary Surgery at NewYork-Presbyterian and Columbia, received a call seeking guidance from a former Columbia trainee who was now leading a transplant center in Texas. One of his team’s patients, Chris Carrales, 54, who had previously undergone a living donor liver transplant, had suffered trauma to his abdomen that led to portomesenteric venous thrombosis: clots in the portal vein that extended into the mesenteric veins, which were disrupting blood flow between the digestive organs and the liver, causing the liver to fail. Attempts by the local care team to address the clotting were unsuccessful, and the outreach to Dr. Kato was a last attempt at treatment.
What followed was nearly a year of preparing Chris for the only solution that could potentially prolong his life: an extremely rare, six-organ multivisceral transplant (MVT) that would require not only another transplant of his liver, but also transplant of the stomach, large intestine, small intestine, pancreas, and kidney.
There are many patients with extensive thrombosis who end up in hospice because physicians may not realize a multivisceral transplant is an option when liver transplantation alone isn’t enough.
— Dr. Tomoaki Kato
The need for multiorgan transplantation was primarily due to the location and diffuse nature of the clotting, which was impacting the splenic vein and superior and inferior mesenteric veins. “If only the upper portion of the portal vein was clotted, we would only need to transplant the liver,” explains Dr. Kato, a pioneer in multiorgan transplantation. “But when clots go down that far, the liver does not receive blood flow from the intestines, and the patient is unable to function. This type of case requires all the organs to be transplanted at once.”
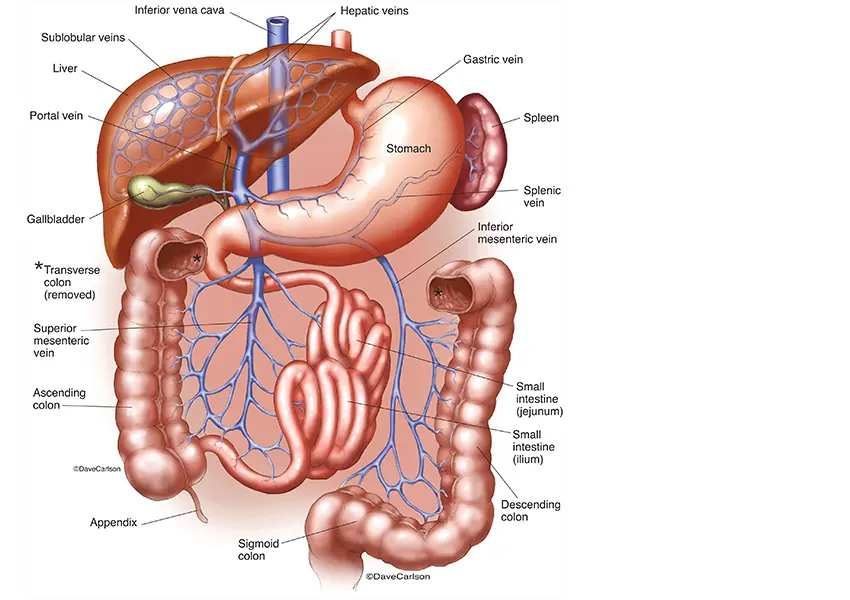
Anatomy of the hepatic portal system. Clotting was present in the portal and splenic veins and the inferior and superior mesenteric veins, preventing proper blood flow to the liver and necessitating a multiorgan transplant.
Stabilization Before Transplantation
Chris flew to New York in November 2023 to undergo more than a week of testing to assess his condition. Due to the lack of blood flow his liver had become cirrhotic, which, along with possible nephrotoxicity caused by antirejection medications taken for his first transplant, were contributing to kidney failure as well. He agreed to the MVT but with his health declining, “we needed to stabilize him first to prepare him for the multivisceral transplant,” says Dr. Kato. “If we couldn’t achieve that, he wouldn’t survive the surgery. There was a significant effort to get him nutritionally better while protecting the liver.”
In February 2024, Chris was transferred from his local hospital to NewYork-Presbyterian and Columbia to begin several months of specialized care to prepare him for transplantation. His multidisciplinary care was led by Mercedes Martinez, M.D., medical director of the Intestinal Transplant Program at the Center for Liver Disease and Abdominal Organ Transplantation at NewYork-Presbyterian, and his care team included physician assistants, nurses, dietitians, nephrologists, gastroenterologists, and physical therapists, among others, who were instrumental to providing the comprehensive care he needed.
Comprehensive, multidisciplinary care before transplantation is essential for short- and long-term survival.
— Dr. Mercedes Martinez
At the time of Chris’ transfer, he had decompensated portal hypertension, requiring drainage of 5 to 6 liters of ascitic fluid twice a week. During his time in the hospital, he also required regular kidney dialysis and frequent paracentesis; intensive nutritional support, including total parental nutrition; and intensive physical rehabilitation due to his severe frailty. “He would not have survived the surgery without the multidisciplinary support,” says Dr. Martinez. “Comprehensive, multidisciplinary care before transplantation is essential for short- and long-term survival.”
By June, he was stable enough to leave the hospital and receive home care while waiting for donor organs — but returned less than two weeks later when the transplant team received the call that both the digestive organs and a kidney had become available from a single deceased donor. “For a multivisceral transplant, all the organs need to come from the same donor because of the immunological advantages that provides,” explains Dr. Kato. On July 6, a surgical team that included Dr. Kato and NewYork-Presbyterian and Columbia transplant surgeons Peter Liou, M.D., Nathaly Llore, M.D., and Joshua Weiner, M.D., along with a transplant fellow, began the operation.
A Complex Surgery Performed Over Multiple Days
There were several challenges that made an already delicate surgery more demanding. Chris had severe abdominal adhesions from his previous liver transplant surgery that made dissection of the organs difficult, even after performing lysis. Additionally, the lesser omentum was completely collapsed, complicating the division of the stomach for removal.
One of the biggest challenges, however, was the bleeding that resulted from how diffuse the thrombosis was throughout the portal system. “Once the vein clots, there is always some venous blood that tries to find a way to get back to the heart through collateral vessels, which makes this type of surgery much more difficult,” explains Dr. Kato.
Administering anesthesia for such an intricate surgery can also prove complicated. “We work very closely with the surgeons to keep up with transfusion requirements while carefully managing acid-base balance and electrolyte disturbances, and while maintaining adequate hemodynamics,” explains Tricia Brentjens, M.D., clinical chief of liver transplant anesthesia services at NewYork-Presbyterian and Columbia. “These cases are exceptionally complex and demand a high level of expertise.”

Patient Chris Carrales, center, with wife, Jessica, and Dr. Kato.
For more than eight hours, the team severed the existing connections, removed the abdominal organs, and transplanted the donor liver, stomach, entire small intestine, pancreas, right kidney and right colon en bloc. Although ultrasound showed strong blood flow and good perfusion, blood loss from the collateral veins made it difficult to complete the surgery — about 24 liters of blood needed to be transfused — so after the surgeons achieved a reasonable level of hemostasis, Chris was sent to the surgical intensive care unit for a day to stabilize.
On July 8, Dr. Kato, Dr. Liou, and Dr. Weiner performed a second surgery to complete any remaining procedures to close vital connections (including an esophagogastrostomy, colocolostomy, and end-to-end right ureteral reconstruction over a stent) and to create a loop ileostomy. A right nephrectomy was also performed to help control bleeding and to allow the allograft kidney to lay in a better position, with the surgeons removing about a liter of blood clots around the kidney. In total, both surgeries took more than 12 hours to complete.
Chris remained in recovery at NewYork-Presbyterian and Columbia for nearly three months post-surgery before being discharged. Several months later he returned to daily activities and maintains regular check-ins and testing with his care team to monitor for rejection and any other issues that may arise as he continues his recovery, with day-to-day post-transplant care led by Monica Velasco, DNP, and Emmanuel Serrano, R.N.
“I’m still regaining my strength, but my improvement has happened in leaps and bounds,” Chris says. “Even though I’m not 100%, I’m still living life, and life is good. I knew that if I just stayed strong that everyone else around me — my entire care team, my wife, my family — would stand behind me and help me get through this.”
“There are many patients with extensive thrombosis who end up in hospice because physicians may not realize MVT is an option when liver transplantation alone isn’t enough,” says Dr. Kato. “While the recovery can be difficult and the patient journey is long, we need to do more in the medical community to raise awareness of MVT and get these patients into specialized programs that have the expertise to manage their highly complex conditions. We should do everything we can to give them the best chance at survival.”










