An artificial intelligence model developed by physicians and data scientists at NewYork-Presbyterian and Weill Cornell Medicine can help predict which pregnant patients are at risk for postpartum depression (PPD), giving obstetricians an opportunity to assess what types of clinical treatment or social services support may be beneficial before symptoms begin.
The model uses routinely collected data contained in a patient’s electronic health record (EHR) to produce a risk score, and those who are at medium or high risk are flagged for physicians in their workflow in Epic, the EHR software platform.
“Postpartum depression is a really underdiagnosed and undertreated disease that affects about 20% of the population, and it can lead to a lot of morbidity,” says Rochelle Joly, M.D., an OB-GYN at NewYork-Presbyterian and Weill Cornell Medicine and the clinical lead on the team that developed the tool. “It typically isn’t diagnosed until symptoms kick in, so preventive therapy is always best.”
“A lot of times, it’s up to the patient to decide how much they want to open up and talk about their mental health. And doctors may not necessarily think to ask questions about it unless the patient brings it up,” says Yiye Zhang, Ph.D., associate professor of population health sciences at Weill Cornell Medicine, whose lab created the risk-assessment algorithm. “We’re hoping this acts as a passive trigger for those conversations to happen.”
Developing the Postpartum Depression Risk Algorithm
Development on the model began in 2018, spurred by a question from one of Dr. Zhang’s students about whether AI could be used to predict PPD. Researchers used the data of more than 15,000 women who were patients at a single NewYork-Presbyterian and Weill Cornell Medicine clinical site between 2015 to 2018 to pinpoint the risk factors, and validated their results against a dataset of nearly 54,000 women who were seen between 2004 to 2017 at a consortium of health organizations; the primary outcome was a PPD diagnosis one year after childbirth. Their findings, which showed that the algorithm could correctly predict which women would go on to develop postpartum depression, was published in the Journal of Affective Disorders in 2020.
If you see the red flag, that can act as a signal to pause and ask additional questions. Nobody has to change the way they manage patients, but the tool provides an extra opportunity to intervene.
— Dr. Rochelle Joly
Thirty key datapoints, which are assessed at regular intervals during pregnancy, were ultimately included in the AI model to help assess risk, including mental health history; demographic information; comorbidities like hypothyroidism and hypertensive disorder; pregnancy complications; prescriptions; vital signs; and health service utilization, such as the number of emergency department visits, which is viewed as an indicator of access to prenatal and primary care.
Throughout development of the clinical tool, the team did extensive work to ensure a user-centered design. They conducted clinician surveys to understand the current workflow and met with departmental leadership to better understand the interventions available for patients at risk and to make sure the tool would be useful for supporting clinical decision-making.
“We did quite a bit of prep to consider how we could change the workflow without disrupting it too much,” Dr. Zhang says. “We wanted to make sure that the information we were giving to providers was something that they could actually work with so we can help making doing the right things for the patient easier.”
AI’s Role in Providing Clinical Decision Support
The ultimate goal is for the risk prediction tool to assist physicians in their treatment decisions — not replace their clinical judgment, Dr. Joly says.
The tool is embedded in the physician schedule and provides a visual warning icon in a separate PPD risk column when patients have medium-to-high risk. When physicians click on the icons, they get a larger view that provides additional details, including the patient’s risk score, which specific risk factors they have, and recommended interventions.
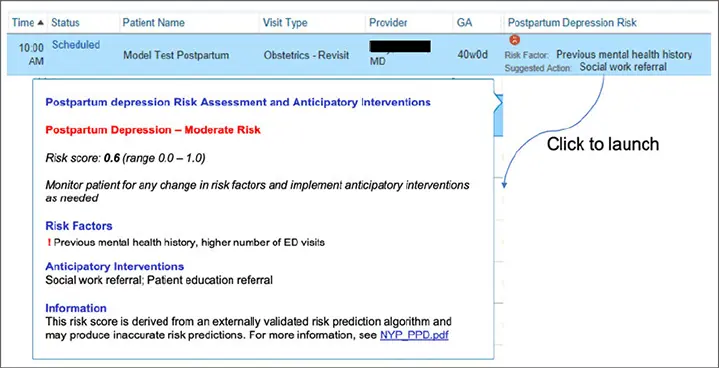
The AI tool provides a visual flag in a physician’s schedule for patients who are at medium to high risk for PPD.
For example, the tool may flag a patient as high risk because they have a history of major depression, in which case a psychiatric referral may make sense. Or they may be suffering from a condition like hyperemesis gravidarum, an extreme form of nausea and vomiting in pregnancy that could affect their mental health, which means medication or other treatment may be more beneficial. When social constraints or a lack of outside support are contributing risk factors, then the physician may consider a referral to a social worker.
“For some patients, the risk factors can be more inconspicuous, and a busy obstetrician may not think to ask about them,” Dr. Joly says. “But if you see the red flag, that can act as a signal to pause and ask additional questions. Nobody has to change the way they manage patients, but the tool provides an extra opportunity to intervene.”
By flagging PPD risk early for all patients regardless of their insurance status, Dr. Joly says the tool also has the potential to expand access to mental health care for underserved patient populations. “The tool is agnostic, so even if someone comes in on the labor floor with no insurance and who has never seen a doctor, they are still going to be flagged for the same risk factors,” she explains. “While they are in the hospital, we then may be able to offer them resources in their zip code that they may not have known about.”
A perinatal wellness program that combines OB-GYN and psychiatric expertise at NewYork-Presbyterian and Weill Cornell Medicine also makes access to mental health treatment easier and more integrated within obstetric care, Dr. Joly adds.
This is really a window of opportunity for us to help moms pay attention to their wellbeing in a way that will lead to better infant outcomes as well. We know from the literature that happier moms lead to healthier babies.
— Dr. Yiye Zhang
Deploying the Tool for Preventive Care
After several years in development, the AI model has now been integrated into the Epic system at three NewYork-Presbyterian and Weill Cornell Medicine women’s health centers, which will help provide data on a diverse patient population. Dr. Joly and Dr. Zhang, along with J. Travis Gossey, M.D., associate chief medical information officer at Weill Cornell Medicine, and obstetrics and gynecology resident Anna Daoud, M.D., MPH, will be conducting an Institutional Review Board-approved randomized clinical trial at these sites to assess physician acceptance of the tool and measure the resulting number of referrals and screenings. “This is really a window of opportunity for us to help moms pay attention to their wellbeing in a way that will lead to better infant outcomes as well,” says Dr. Zhang. “We know from the literature that happier moms lead to healthier babies.”
The tool is also the latest example of how artificial intelligence is making it easier to provide preventive care. “I don’t think of this as the wave of the future anymore, it’s our present reality,” Dr. Joly says. “AI is here to optimize and enhance the delivery of care and to help make care more equitable. The more we use it, the better it’s going to become.”





