Since 2021, NewYork-Presbyterian and Weill Cornell Medicine’s Hyperthermic Intraperitoneal Chemotherapy Treatment Program has offered an innovative procedure for treating peritoneal surface malignancies, when certain cancers — including mesothelioma, colon, appendix, gastric, and primary peritoneal cancers — affect the lining of the peritoneal cavity. The treatment, cytoreductive surgery with hyperthermic intraperitoneal chemotherapy (CRS-HIPEC), involves infusing heated chemotherapy into the abdominal cavity after the removal of all the cancerous tumors.
“The treatment has been used for over two decades and is becoming increasingly recognized as effective for these complex cancers,” says Mehraneh D. Jafari, M.D., chief of colorectal surgery at New York Presbyterian Brooklyn Methodist Hospital and associate program director of Colon and Rectal Surgery at Weill Cornell Medicine. “Since our program was launched, the number of cases we have treated has steadily risen as awareness of this treatment has grown.”
How CRS-HIPEC Works
During cytoreduction, also known as debulking surgery, all visible evidence of disease is removed. Then cannulas are inserted through the same incisions to introduce chemotherapy heated to the temperature of bath water (around 106 to 109 degrees Fahrenheit) into the abdomen. A machine is used to circulate the chemotherapy in and out. “It’s similar to a heart-lung machine, but with just a simple pump and a heating component,” explains Dr. Jafari.
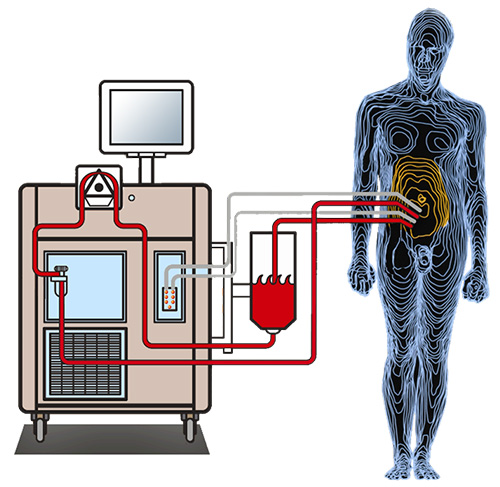
In CRS-HIPEC, cytoreductive surgery is followed by the administration of heated chemotherapy directly to the abdomen to kill any remaining tumor cells in the peritoneal cavity.
The patient’s belly is gently rocked and massaged to allow the chemotherapy to coat the peritoneal surface and kill any microscopic cancer cells. After about an hour and a half, depending on the type of agent used, the solution is drained from the abdomen and the procedure is completed.
Numerous benefits are associated with HIPEC. Heating the chemotherapy enhances its ability to penetrate cancer cells left after surgery. Because the chemotherapy is delivered directly to the abdomen, patients experience fewer side effects than systemic chemotherapy. At the same time, when compared with intravenous administration, HIPEC allows a higher dose of chemotherapy to be used because the body absorbs it differently through the peritoneal walls.
By performing surgery and administering chemotherapy at the same time, we maximize the potential therapeutic effects of both.
— Dr. Mehraneh D. Jafari
“The goal with this comprehensive treatment is to get all the cancer cells out,” says Dr. Jafari. “By performing surgery and administering chemotherapy at the same time, we maximize the potential therapeutic effects of both.”
Patient Selection Criteria for CRS-HIPEC
Currently, cytoreductive surgery and HIPEC is primarily an option for colorectal cancer, appendiceal cancer, peritoneal mesothelioma, pseudomyxoma peritonei, and other rare cancers invading the abdominal cavity. However, recovery can be challenging, so not every patient is a candidate for the treatment, says Dr. Jafari.
The ideal patient has a tumor that has spread only to the peritoneal cavity and not to other organs, such as the liver or lungs. Dr. Jafari’s team looks for certain tumor characteristics that help predict whether the treatment could be beneficial. Colorectal cancer patients who are chosen typically have been on systemic chemotherapy previously and responded well to it.
“It’s best suited for patients without heavy burden of the disease and with low-grade tumors,” Dr. Jafari explains. “And they need to be in otherwise good health to undergo the procedure.”
Potential candidates undergo a diagnostic laparoscopy. Physicians insert a tiny camera into the belly to examine the peritoneal cavity and evaluate the extent of disease. Each case is overseen by a multidisciplinary team, including surgeons, oncologists, pathologists, and radiologists, who discuss it at a tumor board where they develop a personalized treatment plan.
Safety and Efficacy
Complications from the surgery, such as infection, bleeding, or blood clots, occur in an estimated 20% to 30% of patients. Side effects from the chemotherapy are minor when administered directly to the abdomen. Data on the technique has historically been limited but is growing. “It’s difficult to find a large enough cohort of patients that enables you to randomize treatment with CRS-HIPEC versus conventional therapy,” explains Dr. Jafari. “But overall, the treatment has demonstrated acceptable morbidity to the patient population undergoing these procedures.”
In the future, Dr. Jafari hopes to conduct additional research and clinical trials for patients with peritoneal metastases. “The more we can learn about the therapy in a trial setting, the better we may be able to extend this treatment to a broader patient population.”




