$5M
commitment
Sickle Cell Disease (SCD), which affects roughly 100,000 people in the United States, causes red blood cells to form a sickle shape, leading to painful vasoocclusive crises and complications such as stroke, infection, and organ damage. Despite recent medical advances, the median lifespan for individuals with SCD remains just 54 years — far below that of the general population.
In 2025, the Dalio Center conducted a comprehensive assessment of SCD services across NewYorkPresbyterian, engaging multidisciplinary teams at every campus to understand strengths, needs, and gaps in care. This work informed a fiveyear, $5 million plan to enhance SCD services, with investments in social workers, nurse practitioners, and patient coordinators to improve access and continuity of care. The plan also includes funding for projects exploring integrative therapies to support pain management and overall wellbeing.
Our commitment to patient experience continued in 2025 with the second annual Sickle Cell Patient Experience Event, held at the National Basketball Players Association headquarters. More than 100 patients, families, and providers joined the celebration, featuring special guests, including NBA legend John Starks and Brooklyn native Taj Gibson.

Taj Gibson, NBA player, dribbling with a patient during the Sickle Cell Patient Experience Day at the NBPA
Launched in 2024, the CHIPs program was created to elevate and support the ideas of local clinical and operations teams across NewYork-Presbyterian. Recognizing that staff closest to patients and communities often have the most powerful insights into where inequities arise and how to solve them, the Dalio Center designed CHIPs as a mechanism to support locally-driven health equity solutions. With awards of up to $20,000, the program enables local teams to test innovative approaches and drive measurable improvements in care.
After a successful inaugural year, the Dalio Center launched the second CHIPs cycle in June 2025, awarding eight proposals totaling nearly $140,000. Projects began in late 2025 and span a diverse range of equity priorities:

Rebeca Hoey, BSN, RN; Elizabeth Robinson, NP; Bryan Smith, MD; Savannah Pohl, MSW
$140k
grant funding
8
projects
$1.8M
funding
Building on the success of the CHIPs initiative, the Dalio Center developed the PANDA as the next evolution of locally driven, equity-focused innovation. Like CHIPs, PANDA is designed to elevate solutions generated by the teams closest to patient care, but with expanded scope, deeper alignment, and enhanced support.
PANDA brings together diverse project teams from across disciplines and campuses to work toward a single, shared outcome measure. At its core, PANDA is a learning network: teams learn from one another, access guidance from the core PANDA leadership team, and benefit from shared tools, resources, and best practices. The goal is to cultivate a community of likeminded teams across NewYork-Presbyterian collectively advancing health equity through datadriven projects.
In 2025, the Dalio Center launched two networks under this model: the Maternal Health PANDA and the Pediatric PANDA.
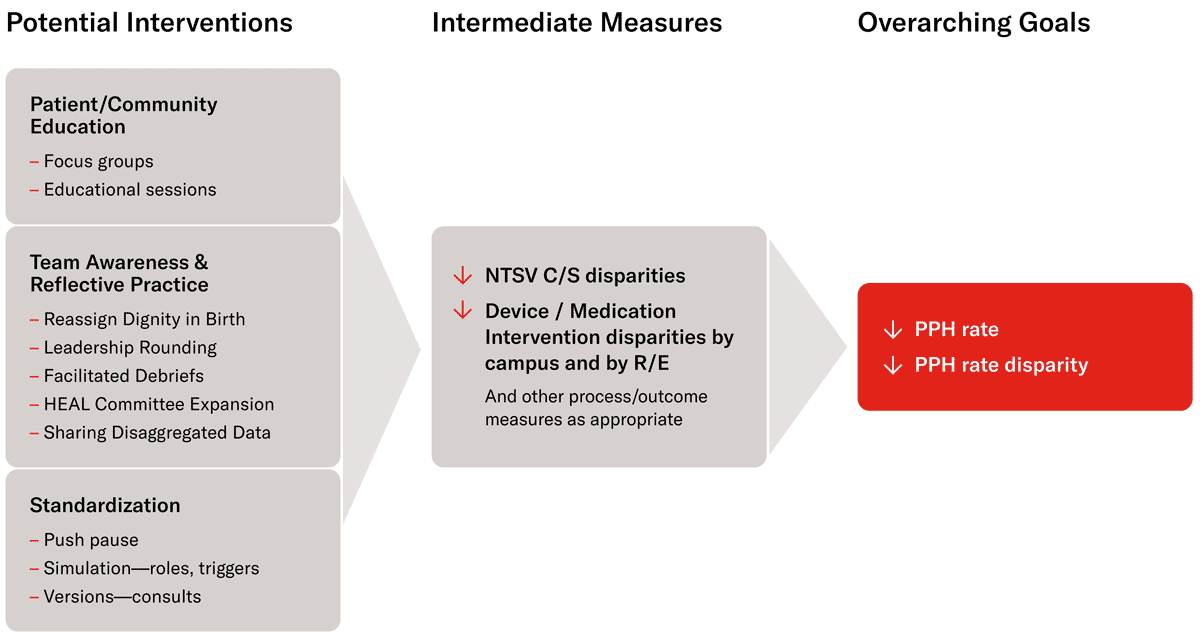
The Dalio Center, in partnership with the Women’s Health Service Line, the Departments of Obstetrics and Gynecology at Weill Cornell Medicine and Columbia University Vagelos College of Physician and Surgeons, and NewYork-Presbyterian’s Department of Quality and Patient Safety launched the Maternal Health PANDA to bring together interventions to reduce disparities in postpartum hemorrhage (PPH). The program awarded $600k in funding over a one-year funding cycle.
The 11 selected projects for the inaugural Maternal Health PANDA include:
The Dalio Center, in partnership with the Children’s Hospital of New York at NewYork-Presbyterian, the Pediatrics Service Line, the Departments of Pediatrics at Weill Cornell Medicine and Columbia University Vagelos College of Physician and Surgeons, and NewYork-Presbyterian’s Department of Quality and Patient Safety launched the Pediatric PANDA to focus on the shared goal of ‘Healthy Kids at Home’. The program awarded over $1.2M in funding over a two-year funding cycle.
The 8 selected projects for the inaugural Pediatric PANDA include:
To address disparities in kidney disease, the Dalio Center partnered with the Rogosin Institute in 2022 to launch an education program at NYP/Columbia University Irving Medical Center and NYP Allen Hospital. With support from the Dalio Center, Columbia University continued the program in 2025, engaging family and caregivers, expanding preemptive transplant counseling, and supporting patients pursuing home dialysis.
The program continues to achieve remarkable success, exceeding national and local averages in pre-emptive transplant rates, home dialysis rates, peripheral vascular access placement, and initiation of dialysis without inpatient admission.
360
patients enrolled in 2025
Cardiovascular health is a key focus for the Dalio Center, with 2025 efforts centered on cardiac sarcoidosis, heart failure, and hypertension. These efforts complement cardiovascular projects described elsewhere in the report, such as the CHIPsfunded heart failure selfmanagement and heart transplant education initiatives, as well as cardiac amyloidosis research supported through the Health Justice Research grants.
Cardiac sarcoidosis is an inflammatory disease in which granulomas form in the heart, disrupting electrical and mechanical function and increasing the risk of arrhythmia and heart failure. Black and African American patients are 2.5 times more likely to develop sarcoidosis and often experience more severe disease and poorer outcomes.
In 2025, an enterprise-wide workgroup of cardiologists and Dalio Center data analysts created a cardiac sarcoidosis registry within our Epic EMR, a standardized outpatient order set, and new patient education materials. Next steps include operationalizing the registry, building a performance dashboard, and advancing patient‑facing educational content.
The Dalio Center is supporting the rollout of a new EMR‑generated heart failure report that identifies patients across eight acute care hospitals who may benefit from a heart failure consultation. The initial phase focuses on using the report to establish baseline data and highlight priority areas for improvement, with the goal of ensuring that all eligible patients receive timely, appropriate care.
Work on hypertension began in 2025 through a partnership with the Ambulatory Quality team. Together, we have been reviewing hypertension control quality measures across primary care sites and have identified several opportunities for improvement. In 2026, the teams will build on this foundation by focusing on improving hypertension management and control across our ambulatory practices, working to close identified equity gaps and strengthen long‑term cardiovascular outcomes.
In May 2024, the Dalio Center funded the launch of the NewYork-Presbyterian Empower program to improve postpartum health outcomes for at-risk individuals, led by Dr. Heather Lipkind, the director of Maternal-Fetal Medicine at Weill Cornell Medicine and a gynecologist-obstetrician at NewYork-Presbyterian/Weill Cornell. In collaboration with the Department of Obstetrics and Gynecology at Weill Cornell, the NewYork-Presbyterian inpatient obstetrics team and the NewYork-Presbyterian Ambulatory Care Network pharmacy team, this initiative provides high risk patients with blood pressure cuffs and education after delivery and clinical pharmacists follow-up remotely with patients to titrate medications.
Preliminary data demonstrate a decrease in emergency department presentations for hypertensive disorders and reduced hypertension-related readmissions among program participants.

Hanlin Li, PharmD, Amber Bradley, PharmD, Jim Thurston, PharmD
81%
of participants engaged in care as of October 2025
The Weill Cornell team has been excellent before and after my pregnancy. I appreciate the team's genuine care for me and my health during our regular check-ins.
My care at Weill Cornell was excellent, and the frequent communication and touchpoints motivated me to keep on top of my health. I felt like everyone I worked with within Weill Cornell really listened to me, cared about my health, and prioritized my wellbeing, which empowered me to manage my own health.
Great team. I love the care and the conversation I was having with the team.
162
unique clients served (as of November 2025)
To improve health outcomes in individuals released from incarceration, TCHR provides comprehensive health services, including primary care, mental health, social work, and obstetrics & gynecology care, along with coordinated referrals to subspecialty services such as dental, orthopedics, cardiology, urology, and rehabilitation medicine. The team also connects patients with community partners for employment, education, legal, and housing assistance.
TCHR employs community health workers with lived experience in the carceral-legal system to support outreach and patient navigation; two returning citizens have been hired into these roles. Since launching in January 2024, TCHR has served 162 unique clients across 452 visits and made 179 subspecialty referrals.
In addition to direct clinical care, TCHR is committed to training the next generation of clinical providers. This includes workshops led by Dr. Alwyn Cohall, professor of public health and pediatrics at Columbia University Vagelos College of Physicians and Surgeons and the Mailman School of Public Health, along with formerly incarcerated clients, to enhance medical students' understanding of mass incarceration, social determinants of health, and their impact on health outcomes in vulnerable communities.

Dr. Alwyn Cohall speaking at the Dalio Center’s Five Year Anniversary Celebration